Can’t Stop Vomiting. Haven’t Peed in Hours. Is This Dehydration Emergency?
You know this feeling. You’ve been sick for hours—maybe days—and no matter how hard you try, you can’t keep anything down. Your mouth feels like sandpaper, your head is pounding, and you’re starting to feel dizzy every time you stand up. You’re already searching “when to go to the ER for dehydration” because something tells you this is getting serious.
Stop. Before you try to drink more water that’s just going to come back up, you need to know something that could change everything about the next few hours.
Here’s what most people don’t realize: By the time you feel severely dehydrated, drinking water often isn’t enough—and sometimes isn’t even possible. When you can’t keep fluids down, when you haven’t urinated in hours, or when you’re feeling confused or faint, your body needs IV fluids that bypass your stomach entirely. Severe dehydration is a medical emergency that requires an ER, not just more Gatorade.
Urgent Care vs. ER: What’s the Actual Difference?
This isn’t about what sign is on the building. It’s about what’s inside the building—and whether they can actually help when dehydration becomes dangerous.
Emergency physicians use a rapid assessment approach to evaluate dehydration severity. You can use the same approach at home.
M — Mental Status: Are you thinking clearly? Can you follow a conversation normally? Warning signs: confusion, disorientation, unusual drowsiness, irritability, difficulty concentrating.
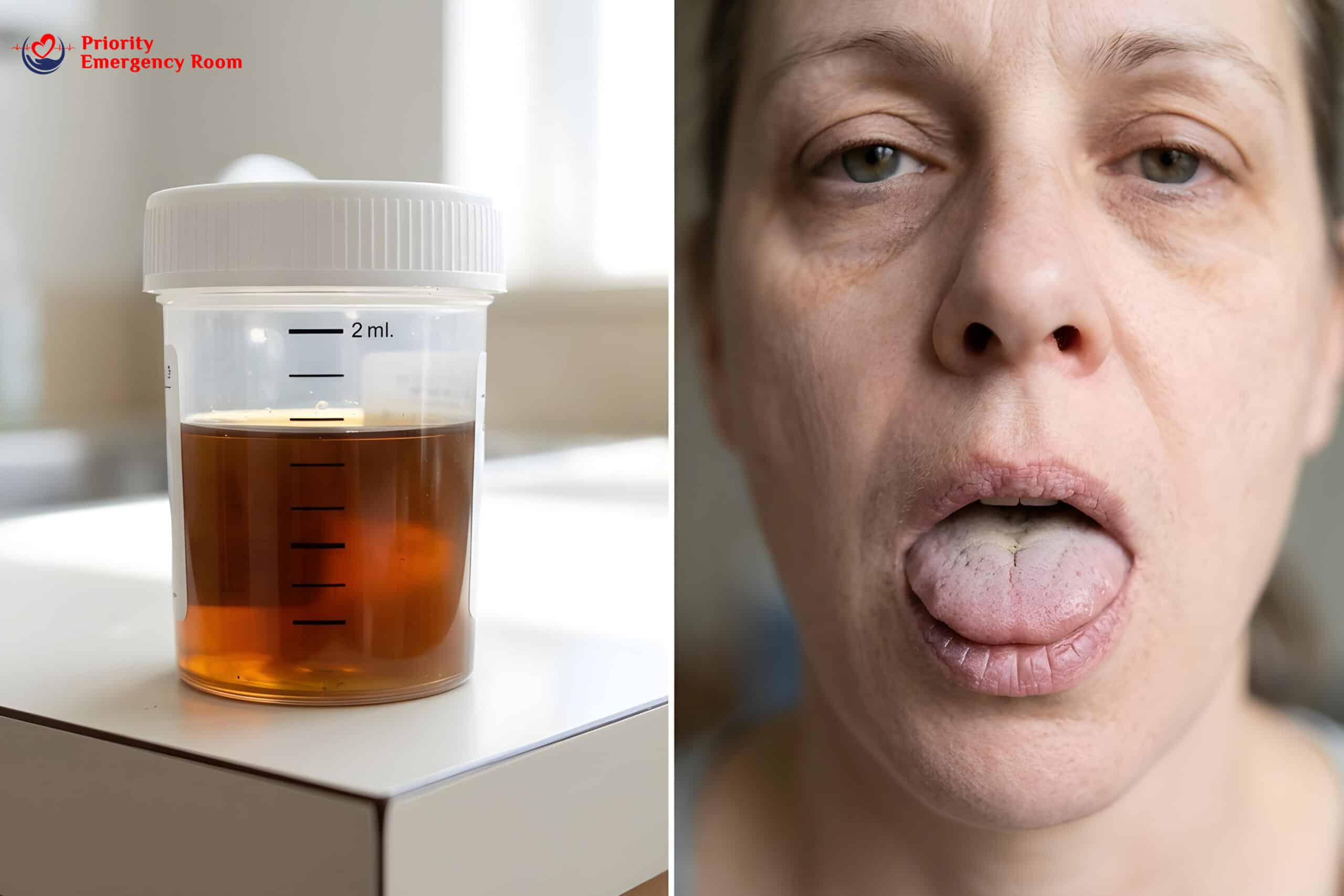
O — Output: Are you urinating at least every 8 hours? Is your urine light yellow? Warning signs: no urination for 8+ hours, very dark or brown urine, no tears when crying (in children).
V — Vitals: Is your heart rate normal? Can you stand without dizziness? Warning signs: rapid heartbeat, dizziness when standing, fainting, sunken eyes, dry cracked lips.
If all three look okay, mild dehydration can often be managed at home. If any one of these looks concerning, seek emergency care immediately.
Many clinics advertise “24 hours” or “extended hours” but actually close at 9 or 10 PM. Before you drive across town at 2 AM, verify they’re actually open. Every Priority ER location is truly open 24 hours a day, 365 days a year—including hot Texas summers when dehydration peaks.
When Home Treatment is Totally Fine
Not every case of dehydration requires the ER. Mild dehydration can often be managed at home with the right approach. Save yourself time and money when the situation calls for it.
Dehydration Situations Appropriate for Home Care
Alert and oriented • Still urinating • Able to keep some fluids down
The key word is mild. When you can still drink, still urinate, and think clearly—home care with oral rehydration can work. But when things escalate, when your body can’t keep up, that’s when you need emergency-level care.
When Dehydration Needs the ER Right Now
Some dehydration is more than just feeling thirsty. There’s a difference between “need more water” and “something’s really wrong.” Trust that instinct. Here’s what our dehydration and vomiting treatment team says warrants immediate ER care:

Emergency
Confusion or Disorientation
Difficulty thinking clearly, confusion about where you are, unusual drowsiness, or difficulty staying awake indicates severe dehydration affecting your brain.
Emergency
No Urination for 8+ Hours
If you haven’t urinated in 8 hours despite trying to drink fluids, your kidneys may not be getting enough blood flow—this can lead to kidney damage.
Emergency
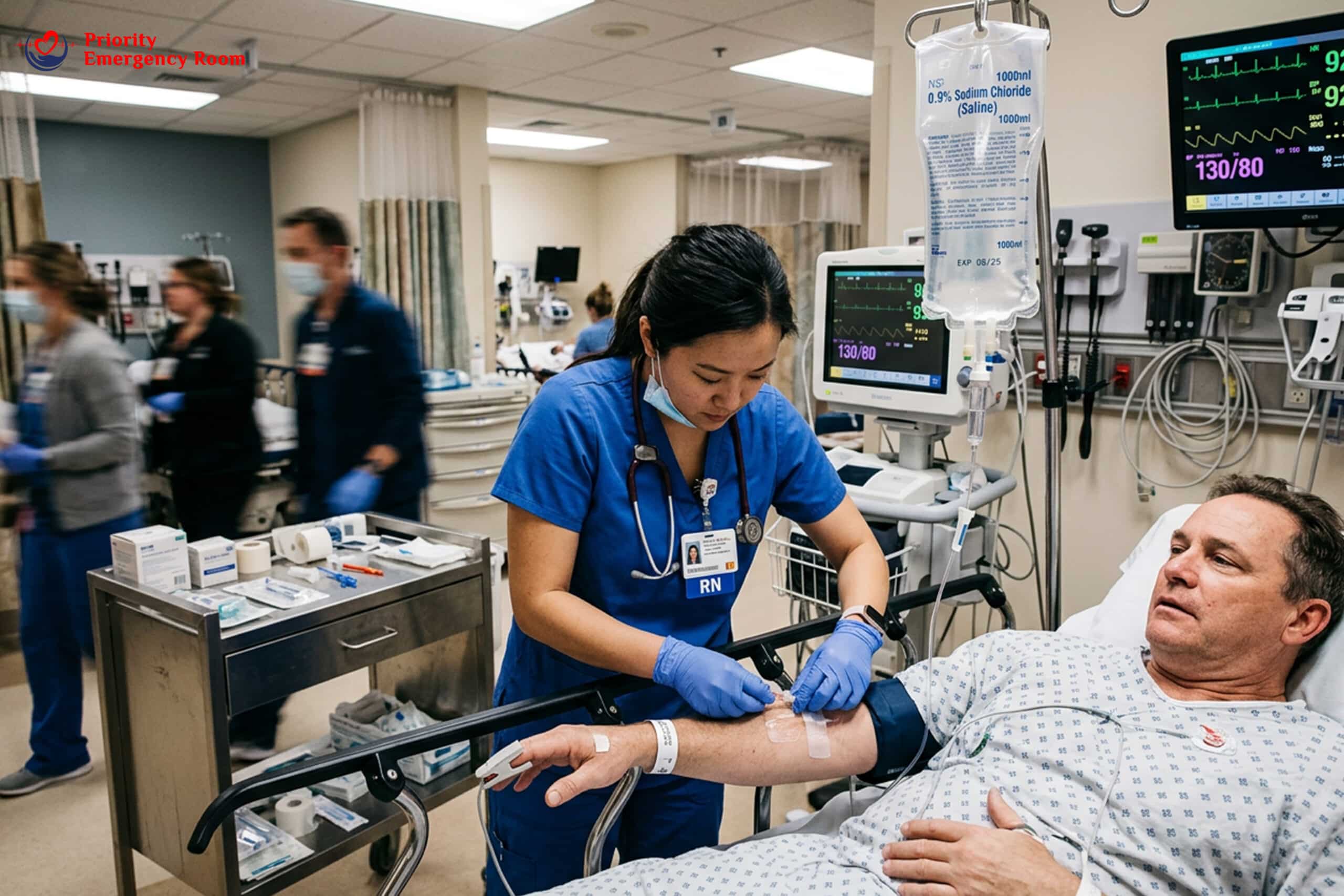
Rapid or Pounding Heartbeat
Your heart racing even at rest is your body’s attempt to compensate for low blood volume. This puts dangerous strain on your cardiovascular system.

Emergency
Fainting or Severe Dizziness
Feeling faint when you stand, actually passing out, or severe lightheadedness means your blood pressure has dropped dangerously low.
Trust Your Instincts
If something feels really wrong—even if you can’t explain why—go to the ER. You know your body better than anyone. That gut feeling exists for a reason.
Built for Reliability When It Matters Most
When dehydration becomes severe and you need IV fluids now, you need certainty—not “maybe” or “we’ll see.” Here’s what makes Priority ER different:
The Difference at 2 AM
Hospital ER
3+ hours
Average wait in Texas
Priority ER
Minutes
Straight to a room
IV Fluids
Started within minutes
Full Lab
Electrolytes & kidney function
Real ER
Board-certified ER physicians
Same capabilities as a hospital ER.
Without the chaos.
What to Expect When You Arrive
Knowing what happens next can help you feel calmer despite how terrible you feel. Here’s how a Priority ER dehydration visit typically unfolds:
Your Priority ER Visit
From arrival to feeling better
0-2 minutes
2-5 minutes
5-15 minutes
15-60 minutes
60-90 minutes
Immediate Greeting (0-2 min)
You’re greeted the moment you walk in. No clipboard, no waiting for someone to notice how terrible you feel.
Private Room (2-5 min)
You go straight to a private treatment room where you can lie down comfortably.
IV Started & Labs (5-15 min)
IV access is established immediately. Fluids start flowing while blood is drawn to check your electrolytes and kidney function.
Fluids & Monitoring (15-60 min)
You receive 1-2 liters of IV fluids while your vital signs are monitored. Anti-nausea medication given if needed.
Feeling Better & Discharge (60-90 min)
Once you’re rehydrated and lab results are reviewed, you’re discharged with instructions for continued recovery at home.
Compare that to a typical hospital ER: wait for triage, wait for a room, wait for IV access, wait for fluids, wait for lab results… You could spend 4-6 hours feeling miserable for the same care that takes 60-90 minutes at Priority ER.²
When Dehydration Needs Emergency Care
Board-certified emergency physicians. Immediate IV fluids. Lab testing for electrolytes and kidney function. Zero wait time. This is what real dehydration emergency care looks like.
Priority ER Locations
All locations are equipped with IV fluid therapy, full laboratory services, and staffed by board-certified emergency physicians ready to treat severe dehydration.
🌵 Odessa (West Texas)
3800 E 42nd St, Suite 105
Odessa, TX 79762
Serving Odessa, Midland, Gardendale, Greenwood & the Permian Basin
🏛 Round Rock (Austin Area)
1700 Round Rock Ave
Round Rock, TX 78681
Serving Round Rock, Cedar Park, Pflugerville, Georgetown & North Austin
⭐ McKinney (North Dallas)
5000 Eldorado Pkwy
McKinney, TX 75072
Serving McKinney, Frisco, Allen, Prosper & Collin County
🏙 Pantego (Arlington)
1607 S Bowen Rd
Pantego, TX 76013
Serving Arlington, Pantego, Grand Prairie & Mid-Cities DFW
🌊 Rockwall (East Dallas)
2265 N Lakeshore Dr #100
Rockwall, TX 75087
Serving Rockwall, Heath, Rowlett, Fate & Lake Ray Hubbard area
The Bottom Line on ER Care for Dehydration
When you’re searching “when to go to the ER for dehydration” while feeling dizzy and unable to keep anything down, you need real answers. Mild dehydration can be treated at home, but severe dehydration—confusion, no urination, rapid heartbeat, fainting—needs IV fluids that only an ER can provide.
Know the difference: if you can sip fluids and still urinate, home care may work. But if you can’t keep anything down, haven’t urinated in hours, or feel confused or faint—you need an ER now. And Priority ER gives you immediate IV access, complete lab work, and treatment—without the chaos and wait times of a hospital ER.
When your body tells you it needs help, trust it. And come to a place that can actually help.
Medical References
- American College of Emergency Physicians. (2024). “Clinical Policy: Critical Issues in the Evaluation and Management of Adult Patients Presenting to the Emergency Department with Acute Dehydration.” ACEP Clinical Policies. Retrieved from https://www.acep.org/
- Centers for Disease Control and Prevention. (2024). “Dehydration.” CDC Health Topics. Retrieved from https://www.cdc.gov/
- National Institute of Diabetes and Digestive and Kidney Diseases. (2024). “Dehydration.” NIDDK Health Information. Retrieved from https://www.niddk.nih.gov/
- American Academy of Pediatrics. (2024). “Dehydration and Diarrhea.” AAP Patient Education. Retrieved from https://www.aap.org/
- Priority ER Internal Data. (2024). “Annual Emergency Department Statistics: Dehydration Presentations.” Quality Assurance Report.
- World Health Organization. (2024). “Diarrheal Disease and Dehydration Treatment.” WHO Guidelines. Retrieved from https://www.who.int/
- Mayo Clinic. (2024). “Dehydration: Diagnosis and Treatment.” Mayo Clinic Patient Care. Retrieved from https://www.mayoclinic.org/
- Healthcare Cost and Utilization Project. (2024). “Emergency Department Visits for Dehydration.” HCUP Statistical Brief. Retrieved from https://hcup-us.ahrq.gov/
- Texas Department of State Health Services. (2024). “Heat-Related Illness Statistics.” Regional Health Report. Retrieved from https://www.dshs.texas.gov/