Dehydration Emergency: When You Need the ER for Fluid Loss
You know something’s wrong. Maybe you’ve been vomiting, had diarrhea, or just haven’t been drinking enough. Now you feel dizzy, your heart is racing, and you can’t seem to catch up no matter how much you try to drink. Is this dehydration serious enough for the emergency room?
Stop. Severe dehydration can affect your heart, kidneys, and brain—and it can become life-threatening. Here’s how to know when dehydration is a true emergency.
Here’s when dehydration becomes an emergency: Go to the ER if you’re confused or disoriented, if your heart is racing, if you feel faint when standing, if you haven’t urinated in 8+ hours, or if you can’t keep fluids down due to vomiting. Severe dehydration requires IV fluids—drinking water isn’t enough when you’re this depleted. The ER can rehydrate you in hours, not days.
Home Hydration vs. ER: What’s the Difference?
Mild dehydration can be treated by drinking more fluids. Severe dehydration requires IV fluids because your body can’t absorb water fast enough through your stomach—and if you’re vomiting, you can’t keep anything down anyway.
Here’s how to assess your dehydration level:
D — Decreased Urination: When did you last urinate? Emergency signs: no urination for 8+ hours, urine that’s very dark or amber colored.
R — Rapid Heart Rate: Is your heart racing? Emergency signs: heart rate over 100 when resting, pounding or racing heartbeat.
Y — Your Mental Status: Are you thinking clearly? Emergency signs: confusion, difficulty concentrating, unusual drowsiness, irritability.
If you have any emergency signs, go to the ER. IV fluids can restore your hydration status in 1-2 hours.
Infants, elderly adults, and people with chronic conditions like diabetes or kidney disease are at higher risk for dangerous dehydration. For infants: no wet diapers for 6+ hours, no tears when crying, or a sunken soft spot are emergencies. For elderly: confusion may be the first sign of severe dehydration. These groups should go to the ER sooner.
When Dehydration Can Be Managed at Home
Mild to moderate dehydration can often be treated at home with oral fluids. Here’s when you can likely manage without the ER.
Dehydration That May Not Need the ER
Keeping fluids down • Urinating regularly • Alert and oriented • No racing heart
The key factor is whether you can keep fluids down. If you’re vomiting everything you drink, or if symptoms aren’t improving despite drinking, you need IV fluids at the ER.
When Dehydration Is an Emergency
These dehydration symptoms require immediate ER care. Don’t wait. Our dehydration treatment team says these need urgent attention:

Emergency
Confusion or Altered Mental State
Difficulty thinking clearly, unusual confusion, excessive drowsiness, or irritability indicates your brain isn’t getting enough fluid. This is serious.
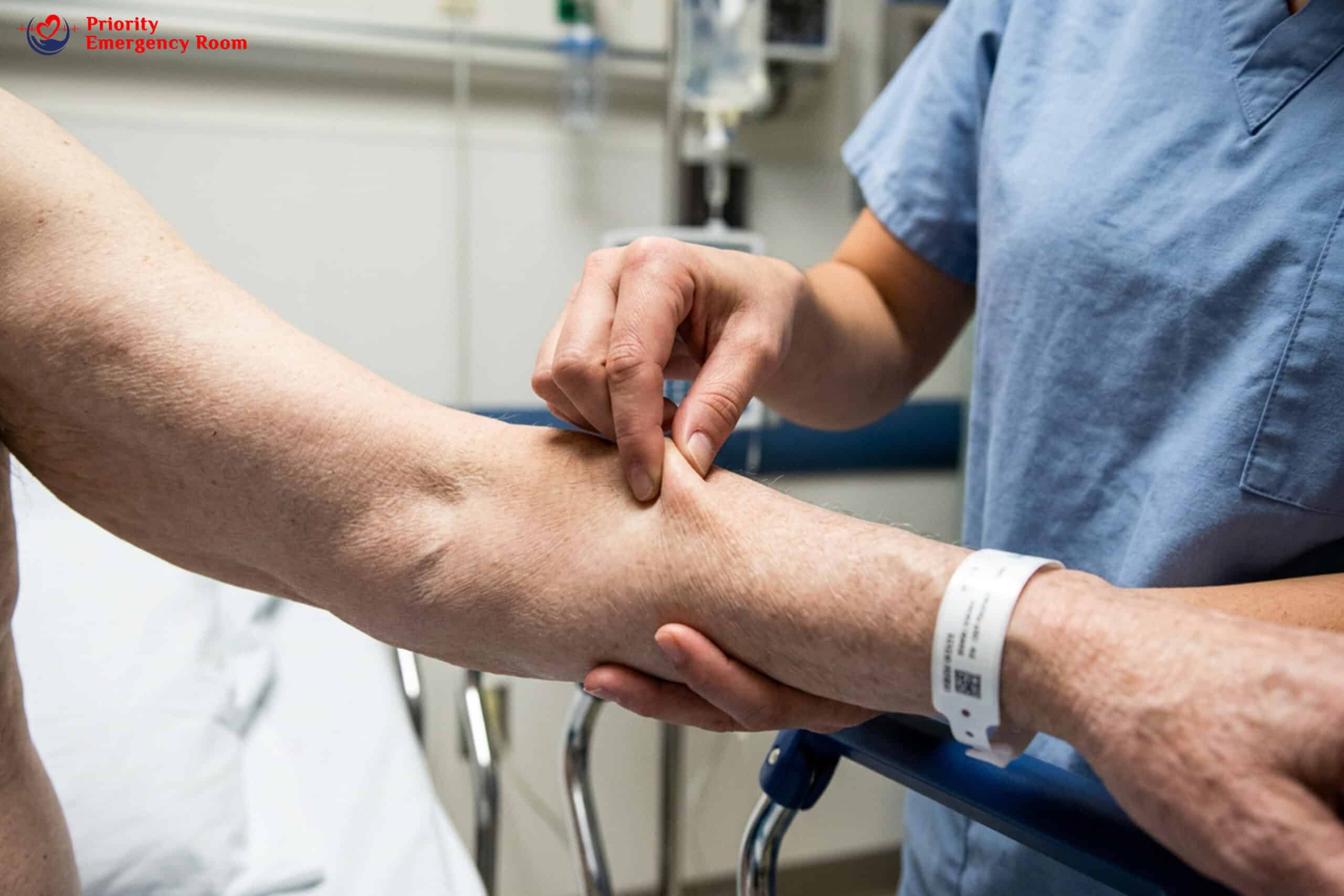
Emergency
Rapid Heart Rate
Heart racing over 100 beats per minute while resting means your heart is compensating for low fluid volume. You need IV fluids.

Emergency
Dizziness or Fainting When Standing
Feeling faint, dizzy, or actually passing out when you stand up indicates your blood pressure is dropping due to fluid loss.
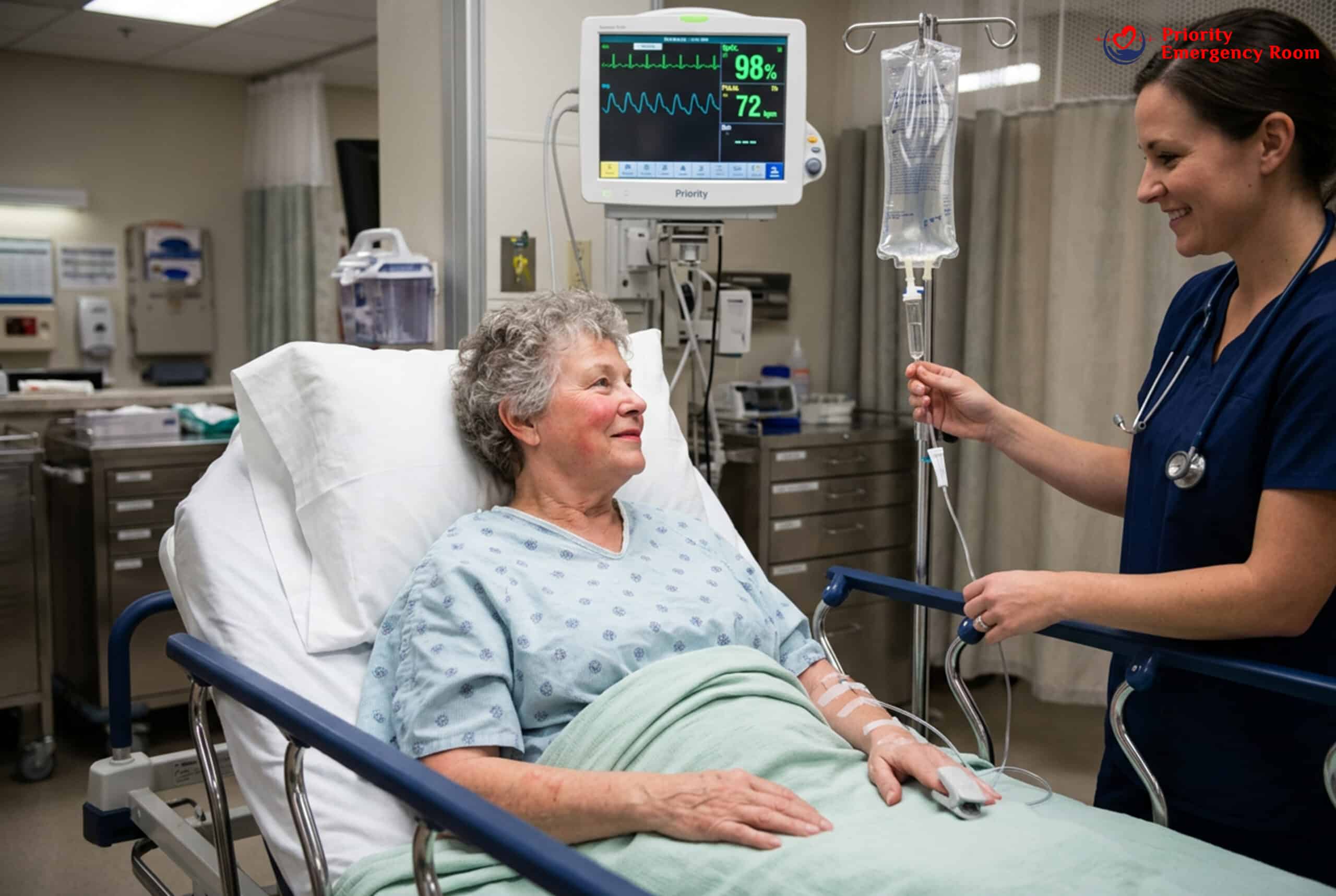
Emergency
No Urination for 8+ Hours
Not urinating for 8 or more hours (or very dark, concentrated urine) means your kidneys aren’t getting enough fluid. This can lead to kidney damage.
Don’t Try to “Tough It Out”
Severe dehydration doesn’t get better just by drinking more water—your body can only absorb so much through your stomach. If you’re showing signs of severe dehydration, IV fluids at the ER can restore your hydration in 1-2 hours instead of days.
Built for Rapid Rehydration
When dehydration becomes an emergency, you need IV fluids fast. Here’s what makes Priority ER different:
The Difference at 2 AM
Hospital ER
3+ hours
Average wait in Texas
Priority ER
Minutes
Straight to a room
IV Fluids
Rapid rehydration
Lab Tests
Electrolyte check
Anti-Nausea
Stop the vomiting
Same capabilities as a hospital ER.
Without the chaos.
What to Expect When You Arrive
Here’s how a Priority ER dehydration visit unfolds:
Your Priority ER Visit
From arrival to rehydrated
0-2 minutes
5-10 minutes
10-15 minutes
15-60 minutes
60-120 minutes
Immediate Greeting (0-2 min)
You’re greeted immediately. No waiting while dehydrated.
IV Started (5-10 min)
IV line placed, fluids begin flowing. Relief starts.
Physician Exam (10-15 min)
Doctor evaluates severity and underlying cause of dehydration.
Labs & Fluids (15-60 min)
Blood tests check electrolytes. 1-2 liters of IV fluid given as needed.
Feeling Better (60-120 min)
Once rehydrated, discharged with instructions for continued recovery.
At Priority ER, IV rehydration begins within minutes of arrival—not hours. Find a 24-hour emergency room near you.²
When Dehydration Becomes Dangerous
Board-certified emergency physicians. IV fluid therapy. Electrolyte testing. Anti-nausea medication. Zero wait time.
Priority ER Locations
All locations have IV fluid therapy, complete laboratory, and board-certified emergency physicians ready to treat dehydration emergencies.
🌵 Odessa (West Texas)
3800 E 42nd St, Suite 105
Odessa, TX 79762
Serving Odessa, Midland, Gardendale, Greenwood & the Permian Basin
🏛 Round Rock (Austin Area)
1700 Round Rock Ave
Round Rock, TX 78681
Serving Round Rock, Cedar Park, Pflugerville, Georgetown & North Austin
⭐ McKinney (North Dallas)
5000 Eldorado Pkwy
McKinney, TX 75072
Serving McKinney, Frisco, Allen, Prosper & Collin County
🏙 Pantego (Arlington)
1607 S Bowen Rd
Pantego, TX 76013
Serving Arlington, Pantego, Grand Prairie & Mid-Cities DFW
🌊 Rockwall (East Dallas)
2265 N Lakeshore Dr #100
Rockwall, TX 75087
Serving Rockwall, Heath, Rowlett, Fate & Lake Ray Hubbard area
The Bottom Line: When Is Dehydration an Emergency?
Dehydration is an emergency when you have confusion, rapid heart rate, dizziness or fainting, no urination for 8+ hours, or can’t keep fluids down. Infants, elderly adults, and those with chronic conditions are at higher risk and should seek care sooner.
Priority ER provides rapid IV fluid therapy and electrolyte testing—everything you need for a dehydration emergency, without the hospital ER wait. When dehydration is caused by severe diarrhea, we can help stop the cycle and restore your fluid balance.
When dehydration becomes dangerous, come get rehydrated fast.
Medical References
- American College of Emergency Physicians. (2024). “Clinical Policy: Dehydration and Fluid Resuscitation.” ACEP. Retrieved from https://www.acep.org/
- Centers for Disease Control and Prevention. (2024). “Dehydration.” CDC Health Topics. Retrieved from https://www.cdc.gov/
- American Academy of Pediatrics. (2024). “Dehydration in Children.” AAP Guidelines. Retrieved from https://www.aap.org/
- World Health Organization. (2024). “Oral Rehydration Therapy.” WHO Guidelines. Retrieved from https://www.who.int/
- Priority ER Internal Data. (2024). “Dehydration Emergency Statistics.” Quality Assurance Report.
- Mayo Clinic. (2024). “Dehydration.” Retrieved from https://www.mayoclinic.org/
- American Geriatrics Society. (2024). “Dehydration in Older Adults.” Retrieved from https://www.americangeriatrics.org/
- Healthcare Cost and Utilization Project. (2024). “ED Visits for Dehydration.” Retrieved from https://hcup-us.ahrq.gov/
- Texas Department of State Health Services. (2024). “Emergency Department Statistics.” Retrieved from https://www.dshs.texas.gov/
