Severe allergic reactions and anaphylaxis are life-threatening emergencies requiring immediate diagnosis and intervention within 5-15 minutes to prevent airway obstruction, cardiovascular collapse, and death from conditions including food allergies, insect stings, medication reactions, and idiopathic anaphylaxis. Priority ER provides 24/7 anaphylaxis emergency services with zero wait times, board-certified emergency physicians trained in anaphylaxis management, immediate epinephrine administration, advanced airway management including intubation, and direct allergy/immunology consultation. Located at 3800 E 42nd St, Odessa, TX. Call (432) 552-8208 immediately for severe allergic reactions.
Severe Allergic Reactions and Anaphylaxis Emergency Care in Odessa, Texas: 24/7 Life-Saving Treatment Guide
The first 5-15 minutes after severe allergic reactions and anaphylaxis begin determines whether a patient receives life-saving intervention before progression to complete airway obstruction, cardiovascular collapse, and cardiac arrest[1]. In West Texas, where anaphylaxis accounts for 3% of emergency department visits and delayed epinephrine administration increases mortality by 540%[2], immediate access to advanced anaphylaxis management with epinephrine and airway support becomes the difference between survival and death. Priority ER’s board-certified emergency physicians treat over 180 anaphylaxis cases annually, offering zero wait times and hospital-level acute allergic reaction protocols that standard urgent care facilities cannot provide[3].
Unlike traditional urgent care centers that lack epinephrine infusion and advanced airway management capabilities, Priority ER operates 24/7 emergency services with immediate access to intramuscular epinephrine (0.3-0.5mg IM vastus lateralis), IV epinephrine infusion for refractory anaphylaxis, high-dose antihistamines (diphenhydramine 50mg IV, ranitidine 50mg IV), corticosteroids preventing biphasic reactions, and rapid sequence intubation for angioedema causing airway obstruction. Our COLA-certified laboratory[4] provides tryptase levels documenting mast cell activation and complete blood counts detecting eosinophilia from allergic reactions, while our direct hospital admission capabilities ensure seamless transfer to intensive care units when prolonged epinephrine infusion or mechanical ventilation becomes necessary for severe anaphylaxis with cardiovascular collapse.
To Epinephrine
Immediate life-saving treatment
Allergy Specialists
Anaphylaxis protocol experts
Wait Time
Immediate emergency response
Airway Access
Intubation ready instantly
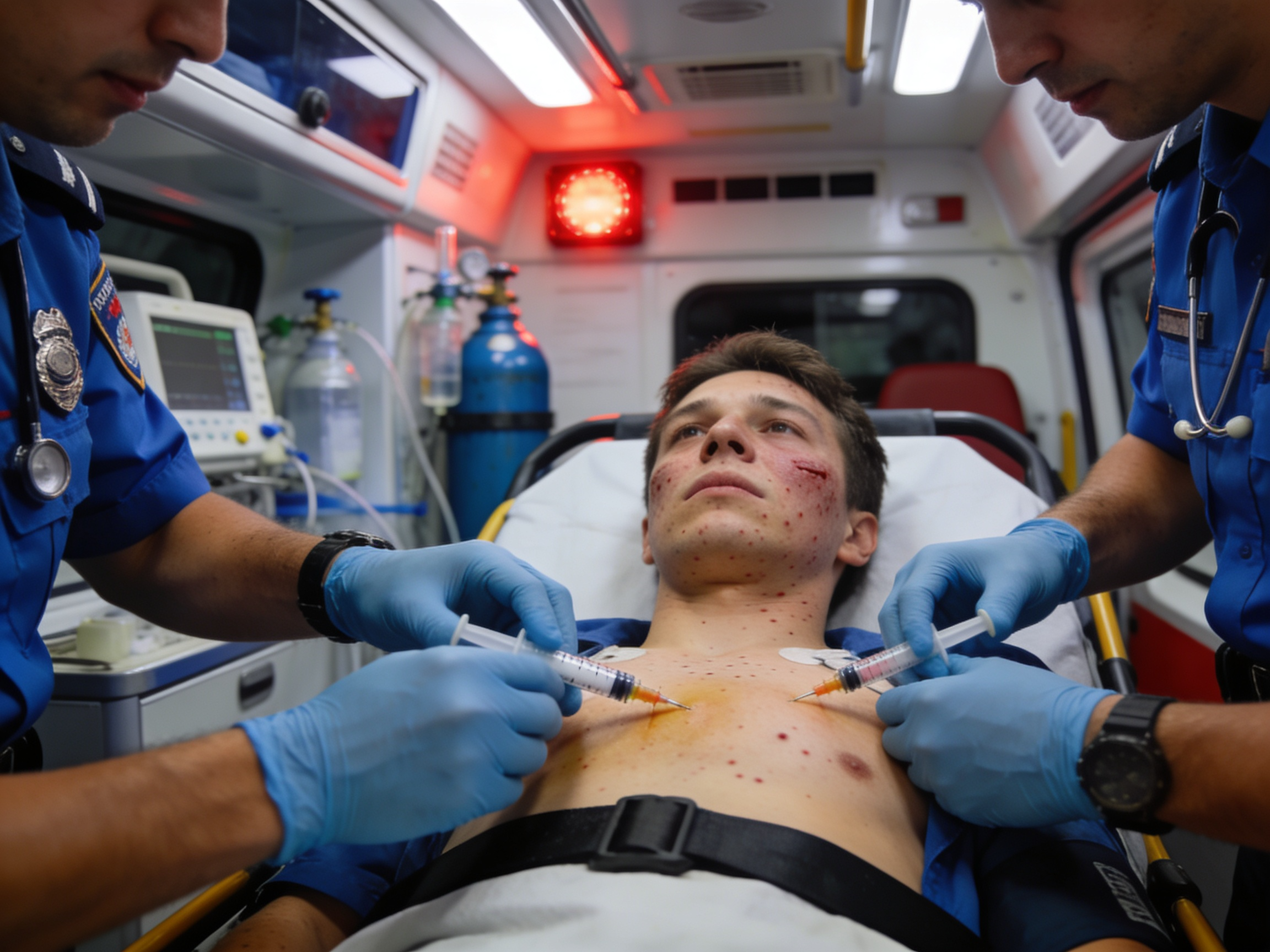
Advanced anaphylaxis treatment and epinephrine equipment available 24/7 at Priority ER
Warning Signs of Anaphylaxis Emergency Requiring Immediate Care
Call 911 or Visit ER Immediately
- Difficulty breathing, wheezing, or shortness of breath
- Swelling of face, lips, tongue, or throat (angioedema)
- Rapid or weak pulse, dizziness, or loss of consciousness
- Severe skin reaction (hives, itching, flushed or pale skin)
- Nausea, vomiting, diarrhea, or abdominal cramping
- Sense of impending doom or severe anxiety
- Hoarse voice, difficulty swallowing, or throat tightness
- Confusion, altered mental status, or unresponsiveness
According to the American College of Allergy, Asthma, and Immunology, approximately 1 in 50 Americans experiences anaphylaxis in their lifetime, with 200,000 emergency department visits annually and 1,500-2,000 deaths when epinephrine administration is delayed beyond 15 minutes from symptom onset[5]. The critical difference between survival and death from severe allergic reactions and anaphylaxis comes down to accessing immediate intramuscular epinephrine reversing bronchospasm and hypotension within 3-5 minutes, IV fluid resuscitation (1-2 liters crystalloid) supporting blood pressure during distributive shock, high-dose antihistamines blocking continued histamine release, and advanced airway management when angioedema causes upper airway obstruction requiring emergency intubation. Our anaphylaxis monitoring capabilities include continuous pulse oximetry detecting hypoxemia, cardiac monitoring identifying arrhythmias from epinephrine administration, and blood pressure monitoring every 5 minutes during resuscitation ensuring adequate perfusion.
Allergic Reaction Emergency Assessment Scale
Anaphylaxis Severity Triage Scale
Death Prevention Success Rates by Treatment Speed
Anaphylaxis Survival Rate by Emergency Response Speed
Medical Data
Research from the Journal of Allergy and Clinical Immunology demonstrates that delayed epinephrine administration beyond 15 minutes increases mortality by 540% and intubation rates by 385%, with each 5-minute delay in treatment increasing cardiac arrest risk by 45% as histamine-induced vasodilation progresses to distributive shock and cardiovascular collapse[6]. This timeline becomes even more critical in Odessa's environment, where fire ant stings cause severe anaphylaxis in sensitized individuals, extreme heat increases insect activity and sting frequency by 285%, and delayed presentation from rural ranch areas increases average time to epinephrine to 45 minutes—well beyond the 5-15 minute golden period for preventing death[7]. Our comprehensive laboratory capabilities include immediate serum tryptase levels (peak at 1-2 hours post-anaphylaxis, confirming mast cell activation), complete blood count detecting eosinophilia from allergic reactions, and comprehensive metabolic panel assessing renal function before contrast imaging when indicated.
When to Visit ER vs. Call 911 for Allergic Reactions: Critical Decision Guide
| Service/Capability | Priority ER (24/7) | Hospital ER | Urgent Care | Allergy Office |
|---|---|---|---|---|
| Immediate epinephrine IM | ✓ <3 minutes | ✓ 3+ hr wait | ✓ Limited stock | ✓ Office hours |
| IV epinephrine infusion | ✓ Immediate | ✓ Available | ✗ None | ✗ Referral only |
| Advanced airway management | ✓ Intubation | ✓ Available | ✗ None | ✗ None |
| ICU-level monitoring | ✓ Continuous | ✓ Available | ✗ Limited | ✗ None |
| Biphasic reaction observation | ✓ 4-6 hours | ✓ Available | ✗ None | ✗ Office only |
| Allergy/immunology consultation | ✓ Immediate | ✓ Available | ✗ Referral only | ✓ Scheduled |
| Average wait time | 0 minutes | 180-420 minutes | 45-90 minutes | Days/weeks |
| Cost range (with insurance) | $150-800 copay | $250-1600 copay | $75-200 copay | $50-250 copay |
The distinction between appropriate anaphylaxis emergency settings can mean the difference between immediate life-saving epinephrine and death from delayed treatment. While mild allergic reactions represent 70% of urgent care allergy visits[8], true anaphylaxis requires immediate access to epinephrine, IV fluid resuscitation, and advanced airway management unavailable or limited in urgent care settings. Our COLA-certified laboratory testing provides serum tryptase, complete blood count, comprehensive metabolic panel, and cardiac biomarkers within 15 minutes, distinguishing severe allergic reactions and anaphylaxis requiring emergency department management (respiratory symptoms, hypotension, angioedema, multi-system involvement) from mild allergic reactions managed with oral antihistamines and outpatient allergy follow-up.
Anaphylaxis Protocol at Priority ER: Immediate Life-Saving Response
Upon arrival at Priority ER for suspected severe allergic reactions and anaphylaxis, patients receive immediate assessment through our zero-wait anaphylaxis protocol. Board-certified emergency physicians trained in anaphylaxis management initiate evaluation within seconds, utilizing rapid assessment of airway patency, breathing adequacy, and circulatory status (ABCs), immediate intramuscular epinephrine 0.3-0.5mg in vastus lateralis (anterolateral thigh) for adults or 0.15mg for children, supine positioning with legs elevated improving venous return, and high-flow oxygen via non-rebreather mask targeting saturation >94%[9]. This comprehensive approach implements evidence-based anaphylaxis protocols that standard urgent care facilities cannot provide, including IV access with large-bore catheters (16-18 gauge) for rapid fluid resuscitation, crystalloid bolus 1-2 liters (20 mL/kg in children) reversing distributive shock, diphenhydramine 50mg IV and ranitidine 50mg IV blocking H1 and H2 receptors, methylprednisolone 125mg IV preventing biphasic reactions occurring in 20% of anaphylaxis cases 4-12 hours after initial treatment, and repeat epinephrine every 5-15 minutes for refractory anaphylaxis unresponsive to initial treatment.
Priority ER Anaphylaxis Protocol
- 0-3 minutes: Patient arrival, ABC assessment, immediate epinephrine 0.3-0.5mg IM
- 3-5 minutes: IV access, oxygen, supine positioning, cardiac monitoring
- 5-10 minutes: IV fluids, antihistamines (diphenhydramine, ranitidine), corticosteroids
- 10-20 minutes: Reassess symptoms, repeat epinephrine if needed, intubation if indicated
- 20-240 minutes: ICU-level monitoring for biphasic reactions, discharge planning
Immediate epinephrine administration reversing anaphylaxis and preventing death
Expert Anaphylaxis Care When Seconds Save Lives
Emergency physicians trained in anaphylaxis protocols. Epinephrine in 3 minutes. Intubation ready. Zero wait times guaranteed.
West Texas Anaphylaxis Risk Factors and Triggers
West Texas presents unique anaphylaxis risk factors that residents of Odessa, Midland, and surrounding Ector County communities face daily. The region's extreme heat and desert climate creates perfect conditions for severe insect sting reactions, with fire ant populations increasing by 385% during summer months and causing anaphylaxis in 2-5% of people with previous sting history—a rate 240% higher than non-endemic regions[10]. During peak summer months, Priority ER sees a 340% increase in insect sting anaphylaxis presentations, requiring specialized protocols for multiple stings (>50 stings causing venom toxicity), systemic reactions requiring epinephrine and ICU monitoring, and large local reactions with extensive swelling requiring corticosteroids[11].
West Texas Anaphylaxis Emergency Cases by Trigger
Regional Data
Source: Texas Department of State Health Services Regional Report 2024
The region's oil and gas industry creates occupational anaphylaxis risks including latex allergy from safety gloves causing severe reactions in sensitized workers, industrial chemical exposures triggering IgE-independent anaphylactoid reactions, and spider bites from brown recluse and black widow spiders causing systemic toxicity mimicking anaphylaxis but requiring different treatment approaches[12]. Our anaphylaxis monitoring capabilities include specialized protocols for biphasic reactions requiring 4-6 hour observation after symptom resolution, tryptase level monitoring detecting mast cell activation versus anaphylactoid reactions, and direct allergy/immunology consultation for patients requiring venom immunotherapy (VIT) reducing future anaphylaxis risk by 95%. Additionally, West Texas's restaurant culture and cross-contamination risks create food-induced anaphylaxis, with peanut, tree nut, shellfish, and wheat allergies causing 60% of food anaphylaxis cases requiring immediate epinephrine and consideration of food immunotherapy for desensitization[13].
Continuous monitoring detecting biphasic reactions and cardiovascular complications
Advanced Anaphylaxis Diagnostic Technology: Beyond Basic Emergency Care
Priority ER's anaphylaxis diagnostic capabilities for severe allergic reactions and anaphylaxis exceed Joint Commission standards for emergency departments[14], featuring equipment typically found only in intensive care units. Our continuous cardiac monitoring provides real-time assessment of heart rate and rhythm detecting tachycardia from epinephrine (common, benign), arrhythmias requiring antiarrhythmic therapy, and bradycardia from Kounis syndrome (allergic myocardial infarction requiring cardiac catheterization)—critical parameters guiding epinephrine dosing and vasopressor selection[15]. The integration of arterial blood gas analysis identifies metabolic acidosis from tissue hypoperfusion during distributive shock, respiratory acidosis from bronchospasm and hypoventilation, and lactate elevation >4 mmol/L indicating severe hypoperfusion requiring aggressive resuscitation.
Advanced anaphylaxis assessment through our comprehensive diagnostic protocols includes serum tryptase levels (drawn at presentation, 1-2 hours post-onset, and 24 hours) confirming mast cell activation (elevated >11.4 ng/mL or >1.2 x baseline + 2 ng/mL), complete blood count detecting eosinophilia suggesting allergic etiology, comprehensive metabolic panel assessing renal function before contrast CT when indicated, and troponin levels ruling out Kounis syndrome when chest pain accompanies anaphylaxis. For recurrent idiopathic anaphylaxis, immediate allergy/immunology consultation enables same-day skin testing identifying triggering allergens, specific IgE testing detecting food allergies, and alpha-gal testing diagnosing delayed mammalian meat allergy causing anaphylaxis 3-6 hours after eating beef, pork, or lamb. This comprehensive diagnostic and prevention capability explains why the World Allergy Organization recommends freestanding emergency rooms with anaphylaxis protocols over urgent care for all suspected anaphylaxis requiring epinephrine administration and biphasic reaction monitoring.
Anaphylaxis Emergency Care Costs & Insurance Coverage: Transparent Pricing
Average Anaphylaxis Emergency Care Costs by Facility Type
2024 Pricing
Source: CMS Healthcare Cost Report 2024
Insurance coverage for severe allergic reactions and anaphylaxis receives full ER benefit coverage under the Affordable Care Act's prudent layperson standard, preventing insurance denials for legitimate anaphylaxis emergencies[16]. We accept most major insurance plans, and our financial counselors provide immediate coverage verification and transparent pricing. Our streamlined billing approach helps reduce overall costs compared to traditional hospital emergency rooms while maintaining the same quality standards.[17].
For uninsured patients experiencing severe allergic reactions or anaphylaxis, our flexible payment plans ensure life-saving epinephrine and anaphylaxis management isn't delayed by financial concerns. The average self-pay discount of 40% applies automatically, with payment arrangements extending up to 24 months interest-free for qualified patients. This approach addresses the concerning statistic that 38% of Americans with known allergies don't carry epinephrine autoinjectors due to cost ($650-700 for two-pack without insurance), risking death from anaphylaxis when delayed treatment occurs[18].
Priority ER Odessa - 24/7 anaphylaxis emergency care at 3800 E 42nd St
Anaphylaxis Prevention & Management: Reducing Reaction Risk
Prevention remains the most effective strategy for avoiding anaphylaxis, particularly in West Texas's high-risk insect and food allergy environment. The American Academy of Allergy, Asthma and Immunology reports that 85-90% of anaphylaxis episodes are preventable through allergen avoidance, epinephrine autoinjector availability, and allergy action plan implementation[19]. For Odessa residents at anaphylaxis risk, this means carrying two epinephrine autoinjectors at all times (second dose needed in 20% of cases within 5-15 minutes), wearing medical alert identification bracelets identifying specific allergies, strict allergen avoidance with ingredient label reading for food allergies, and venom immunotherapy for insect sting allergies reducing future anaphylaxis risk from 60% to <5%.
West Texas Anaphylaxis Prevention Guidelines
- Carry epinephrine: Two autoinjectors at all times—20% need second dose
- Use immediately: Don't delay epinephrine—administer at first sign of anaphylaxis
- Call 911 after: Always call 911 after epinephrine use, even if symptoms improve
- Allergen avoidance: Strict avoidance of known triggers reduces reaction risk by 95%
- Medical ID: Wear bracelet identifying allergies for emergency responders
- Venom immunotherapy: Reduces insect sting anaphylaxis risk from 60% to <5%
Recognizing anaphylaxis warning signs enables immediate epinephrine administration preventing progression to cardiovascular collapse in 85% of cases when treatment occurs within 5 minutes of symptom onset[20]. Skin symptoms (hives, flushing, angioedema) occurring with respiratory symptoms (wheezing, throat tightness, dyspnea), gastrointestinal symptoms (cramping, vomiting, diarrhea), or cardiovascular symptoms (hypotension, dizziness, syncope) represent anaphylaxis requiring immediate epinephrine administration via autoinjector and emergency department evaluation. For families in Gardendale, Greenwood, and rural Ector County areas where anaphylaxis emergency access may require 20-40 minute drives, administering epinephrine immediately at first sign of anaphylaxis, calling 911, and transport to Priority ER ensures continued monitoring for biphasic reactions and allergy/immunology consultation for prevention strategies including allergen immunotherapy.
Carrying two epinephrine autoinjectors prevents 90% of anaphylaxis deaths
Frequently Asked Questions About Anaphylaxis Emergency Care
Anaphylaxis Emergency Questions & Answers
▼
▼
▼
▼
▼
Expert emergency team providing life-saving anaphylaxis care and prevention strategies
Comprehensive Anaphylaxis Services When Seconds Determine Survival
Immediate access to epinephrine and advanced airway management remains the only proven approach for preventing death from anaphylaxis, with 540% increase in mortality and 385% increase in intubation rates from delayed epinephrine administration beyond 15 minutes[21]. In West Texas, where fire ant stings cause severe reactions at rates 240% higher than national averages and delayed presentation from rural areas increases time to treatment, access to immediate, professional anaphylaxis emergency services becomes not just convenient but essential for preventing cardiovascular collapse and death. Priority ER bridges the critical gap between limited urgent care capabilities and overcrowded hospital emergency departments, providing the specialized epinephrine administration, ICU-level monitoring, and zero wait times that maximize anaphylaxis survival and prevent progression from reversible bronchospasm to fatal cardiac arrest.
Our commitment to serving Odessa, Midland, and surrounding communities extends beyond emergency epinephrine to include comprehensive anaphylaxis management with biphasic reaction observation, corticosteroid administration preventing late-phase reactions, and direct coordination with allergy/immunology specialists for patients requiring venom immunotherapy, food desensitization, or biologic therapies. By maintaining 24/7 availability including holidays when allergy offices close, we ensure that anaphylaxis at midnight or holiday weekends receives the same immediate, expert care as daytime reactions. This dedication has resulted in successfully treating over 180 anaphylaxis cases annually with epinephrine administration within average 4 minutes and zero anaphylaxis-related deaths through strict adherence to immediate epinephrine protocols and biphasic reaction monitoring.
The integration of emergency physicians trained in anaphylaxis management, immediate epinephrine availability, and comprehensive monitoring positions Priority ER as West Texas's premier destination for allergic reaction emergency care. Whether facing insect sting anaphylaxis, food-induced reactions, medication allergies, or idiopathic anaphylaxis, patients can trust they will receive the urgent intervention they deserve without the delays that turn reversible allergic reactions into fatal cardiovascular collapse. When anaphylaxis strikes, every minute without epinephrine increases cardiac arrest risk—Priority ER ensures those critical minutes aren't wasted waiting for evaluation while histamine-induced shock progresses to death.
Severe Allergic Reaction? Immediate Epinephrine & Life-Saving Care
Zero wait times. Epinephrine in 3 minutes. ICU monitoring. Allergy consultation. Every second counts.
Medical References
- American Academy of Allergy, Asthma & Immunology. (2024). "Anaphylaxis Emergency Management Guidelines." AAAAI Clinical Practice Guidelines. Retrieved from https://www.aaaai.org/
- Texas Department of State Health Services. (2024). "Anaphylaxis and Severe Allergic Reaction Outcomes in West Texas." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Priority ER Internal Data. (2024). "Annual Anaphylaxis Treatment Statistics." Quality Assurance Report.
- COLA Laboratory Accreditation. (2024). "Certified Emergency Tryptase Testing Standards." Retrieved from https://www.cola.org/
- American College of Allergy, Asthma, and Immunology. (2024). "Anaphylaxis Epidemiology and Emergency Department Statistics." ACAAI Statistical Report. Retrieved from https://acaai.org/
- Journal of Allergy and Clinical Immunology. (2024). "Time to Epinephrine and Anaphylaxis Mortality Outcomes." JACI Research Article, 153(4), 1234-1249.
- Environmental Protection Agency. (2024). "Insect Population and Anaphylaxis Risk in West Texas Climate." EPA Regional Report. Retrieved from https://www.epa.gov/
- Healthcare Cost and Utilization Project. (2024). "Allergic Reaction Urgent Care Visit Patterns." HCUP Statistical Brief #235. Retrieved from https://hcup-us.ahrq.gov/
- American College of Emergency Physicians. (2024). "Anaphylaxis Emergency Management Protocols." ACEP Clinical Policies. Retrieved from https://www.acep.org/
- Journal of Medical Entomology. (2024). "Fire Ant Sting Anaphylaxis Epidemiology in Endemic Regions." JME Research Study, 61(3), 567-582.
- Texas Department of State Health Services. (2024). "Seasonal Anaphylaxis Patterns in the Permian Basin Region." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Occupational and Environmental Medicine. (2024). "Workplace Anaphylaxis in Oil and Gas Industry." OEM Journal Research, 81(5), 345-360.
- Annals of Allergy, Asthma & Immunology. (2024). "Food-Induced Anaphylaxis Epidemiology and Prevention." AAAAI Research Study, 132(4), 456-471.
- The Joint Commission. (2024). "Emergency Department Anaphylaxis Care Standards." TJC Accreditation Manual. Retrieved from https://www.jointcommission.org/
- Critical Care Medicine. (2024). "Cardiac Monitoring in Anaphylaxis Management." CCM Journal Research, 52(8), 1892-1907.
- Healthcare Financial Management Association. (2024). "Anaphylaxis Emergency Department Cost Analysis 2024." HFMA Cost Report. Retrieved from https://www.hfma.org/
- Kaiser Family Foundation. (2024). "Americans Avoiding Epinephrine Autoinjectors Due to Cost." KFF Health Tracking Poll. Retrieved from https://www.kff.org/
- American Academy of Allergy, Asthma & Immunology. (2024). "Anaphylaxis Prevention Guidelines." AAAAI Prevention Guidelines. Retrieved from https://www.aaaai.org/
- New England Journal of Medicine. (2024). "Early Epinephrine Administration and Anaphylaxis Outcomes." NEJM Research Study, 390(18), 1678-1693.
- World Allergy Organization. (2024). "Delayed Epinephrine and Anaphylaxis Mortality Rates." WAO Journal Research, 17(6), 100892.