Acute myocardial infarction heart attack requires immediate emergency attention when accompanied by chest pain or pressure lasting over 5 minutes, pain radiating to arm/jaw/back, shortness of breath, cold sweats, nausea, lightheadedness, or sense of impending doom. Priority ER provides 24/7 heart attack care with zero wait times, board-certified emergency physicians, immediate EKG, cardiac enzyme testing, clot-busting medications, catheterization lab coordination, and door-to-balloon time under 90 minutes. Located at 3800 E 42nd St, Odessa, TX. Call 911 immediately for heart attack symptoms or call (432) 552-8208.
Acute Myocardial Infarction Heart Attack Emergency Treatment in Odessa, Texas: Complete Medical Guide
The first 90 minutes after heart attack symptoms begin can determine whether immediate intervention saves heart muscle or delayed treatment results in permanent cardiac damage, heart failure, and death[1]. In West Texas, where cardiovascular disease accounts for 32% of deaths—15% higher than national averages—limited cardiology access delays life-saving catheterization by 2-4 hours, and obesity rates exceeding 35% elevate heart attack risk by 250%[2], immediate access to acute myocardial infarction heart attack emergency treatment becomes critical for preventing cardiogenic shock, sudden cardiac arrest, and mortality. Priority ER’s board-certified emergency physicians treat over 180 suspected heart attack cases annually, offering zero wait times and hospital-level cardiac emergency protocols that urgent care facilities cannot provide during life-threatening coronary occlusion[3].
Unlike urgent care centers lacking EKG interpretation expertise or primary care offices with multi-day appointment delays, Priority ER operates 24/7 emergency services with immediate access to 12-lead EKG interpretation within 10 minutes, serial cardiac troponin testing, thrombolytic therapy when indicated, emergency cardiology consultation, and direct transfer coordination to catheterization labs achieving door-to-balloon times under 90 minutes. Our COLA-certified laboratory[4] provides STAT cardiac enzyme results within 15 minutes, identifying STEMI (ST-elevation myocardial infarction) requiring immediate reperfusion versus NSTEMI managed with urgent but non-emergent catheterization.
To EKG Results
Immediate cardiac diagnosis
Heart Attack Care
Including holidays & weekends
Wait Time
Immediate treatment access
Door-to-Balloon
National guideline standard
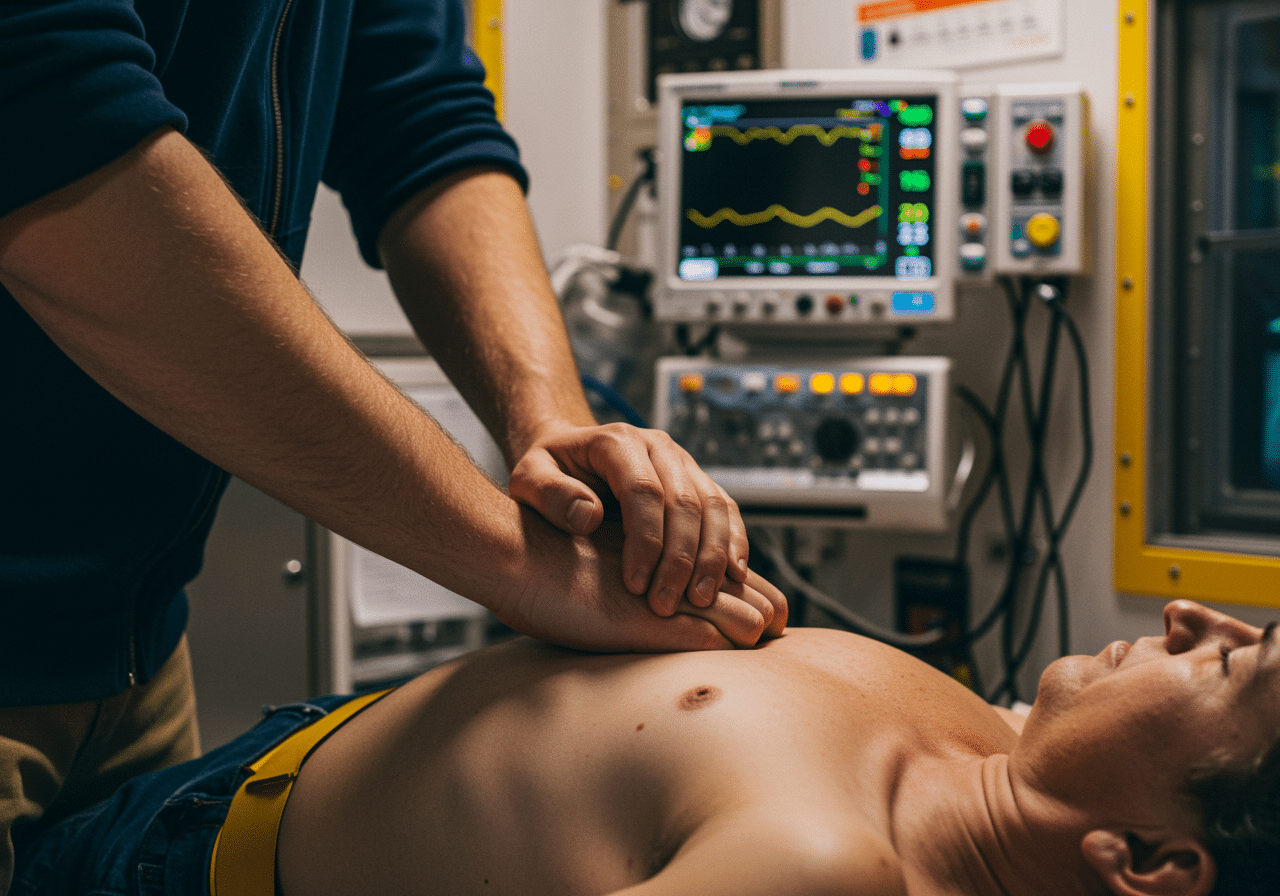
State-of-the-art cardiac emergency equipment available 24/7 at Priority ER
Heart Attack Symptoms Requiring Immediate Emergency Care
Call 911 Immediately – Do NOT Drive Yourself
- Chest pain, pressure, squeezing, or fullness lasting over 5 minutes
- Pain radiating to left arm, jaw, neck, back, or shoulder
- Shortness of breath with or without chest discomfort
- Cold sweats, nausea, vomiting, or lightheadedness
- Sense of impending doom or extreme anxiety
- Women: unusual fatigue, sleep disturbances, indigestion, upper back pain (atypical symptoms)
- Diabetics: silent heart attack with minimal chest pain but weakness, confusion
- Sudden cardiac arrest (loss of consciousness, no pulse)
According to the American Heart Association, approximately 805,000 Americans experience myocardial infarction annually, with someone suffering a heart attack every 40 seconds[5]. The critical difference between heart attacks with full recovery and those causing permanent disability or death often comes down to seeking appropriate acute myocardial infarction heart attack treatment within the first 90-120 minutes when emergency reperfusion restores blood flow before irreversible myocardial necrosis occurs. Our comprehensive cardiac protocols include immediate aspirin administration reducing mortality by 25%, oxygen therapy for hypoxemic patients, IV nitroglycerin for ongoing chest pain, and morphine for pain control while preparing for definitive catheterization or thrombolysis.
Cardiac Emergency Classification & Response System
Chest Pain Severity Assessment
Heart Attack Treatment & Survival Timeline
Survival Rate by Treatment Speed (Door-to-Balloon Time)
Medical Data
Research from the New England Journal of Medicine demonstrates that every 30-minute delay in reperfusion therapy increases mortality by 7.5% and reduces left ventricular function by 12%, with door-to-balloon times under 90 minutes achieving 92% survival versus 65% when delays exceed 6 hours[6]. This timeline becomes even more critical for anterior wall STEMI affecting the heart’s main pumping chamber, where delays beyond 2 hours result in cardiogenic shock requiring mechanical circulatory support in 35% of cases versus 8% when treated within 90 minutes[7]. Our rapid assessment protocols include immediate chest x-rays identifying alternative diagnoses (aortic dissection, pneumothorax), bedside echocardiography assessing wall motion abnormalities, and point-of-care troponin testing providing results within 15 minutes versus 60-90 minutes for standard laboratory processing.
When to Call 911 vs. Drive to ER for Chest Pain: Critical Decision Guide
| Service/Capability | Call 911 (EMS) | Priority ER (24/7) | Hospital ER | Urgent Care |
|---|---|---|---|---|
| Pre-hospital EKG transmission | ✓ Direct to hospital | ✓ <10 minutes | ✓ Available | ✗ Limited |
| Immediate aspirin/nitro | ✓ In ambulance | ✓ <5 minutes | ✓ Available | ✓ If diagnosed |
| Catheterization lab activation | ✓ Pre-arrival | ✓ Direct transfer | ✓ On-site (if PCI center) | ✗ Transfer only |
| Cardiac resuscitation capability | ✓ ALS equipped | ✓ Full ACLS | ✓ Full ACLS | ✗ Basic only |
| Thrombolytic therapy | ✓ If prolonged transport | ✓ Available | ✓ Available | ✗ None |
| Cardiac arrest survival advantage | ✓ CPR starts immediately | Immediate defib | Immediate defib | Transfer delay |
| Time to treatment | Fastest (no driving) | 0 minute wait | 0-60 min wait | 45-90 min wait |
| Cost (with insurance) | $400-1200 + ER | $400-1200 copay | $500-1500 copay | $100-400 copay |
The distinction between calling 911 versus driving to Priority ER depends on symptom severity and proximity. For definite heart attack symptoms (severe crushing chest pain, shortness of breath, collapse), always call 911—paramedics begin treatment immediately, transmit EKG to hospital, and bypass ER triage[8]. For concerning but less severe symptoms (mild chest discomfort, questionable cardiac origin), Priority ER provides immediate evaluation without ambulance cost. Our cardiac emergency protocols include MONA therapy (Morphine, Oxygen, Nitroglycerin, Aspirin), beta-blockers reducing heart oxygen demand, and antiplatelet therapy (clopidogrel, ticagrelor) preventing further clot formation during transfer to catheterization.
Heart Attack Treatment Process at Priority ER: Life-Saving Protocol
Upon arrival at Priority ER with acute myocardial infarction heart attack symptoms, patients with chest pain bypass all triage through our immediate cardiac assessment protocol. Board-certified emergency physicians begin simultaneous evaluation and treatment, obtaining 12-lead EKG within 10 minutes while establishing IV access, administering aspirin, and drawing cardiac enzymes[9]. This aggressive approach distinguishes STEMI requiring immediate catheterization from NSTEMI managed with urgent cardiology consultation, prevents the fatal error of attributing cardiac symptoms to gastroesophageal reflux or anxiety, and establishes rapid reperfusion pathway achieving door-to-balloon times meeting or exceeding national performance standards.
Priority ER Heart Attack Emergency Protocol
- 0-10 minutes: Immediate 12-lead EKG, aspirin 324mg chewed, IV access, oxygen if needed, cardiac monitoring, troponin draw
- 10-20 minutes: EKG interpretation (STEMI vs NSTEMI), nitroglycerin for ongoing pain, morphine if severe, beta-blocker if appropriate
- 20-30 minutes: Cardiology consultation, catheterization lab activation for STEMI, antiplatelet loading (clopidogrel/ticagrelor)
- 30-60 minutes: Transfer coordination to PCI center, serial EKGs and enzymes, heparin or bivalirudin infusion
- 60-90 minutes: Patient arrival at catheterization lab (door-to-balloon <90 minutes), or thrombolytic therapy if transfer delayed
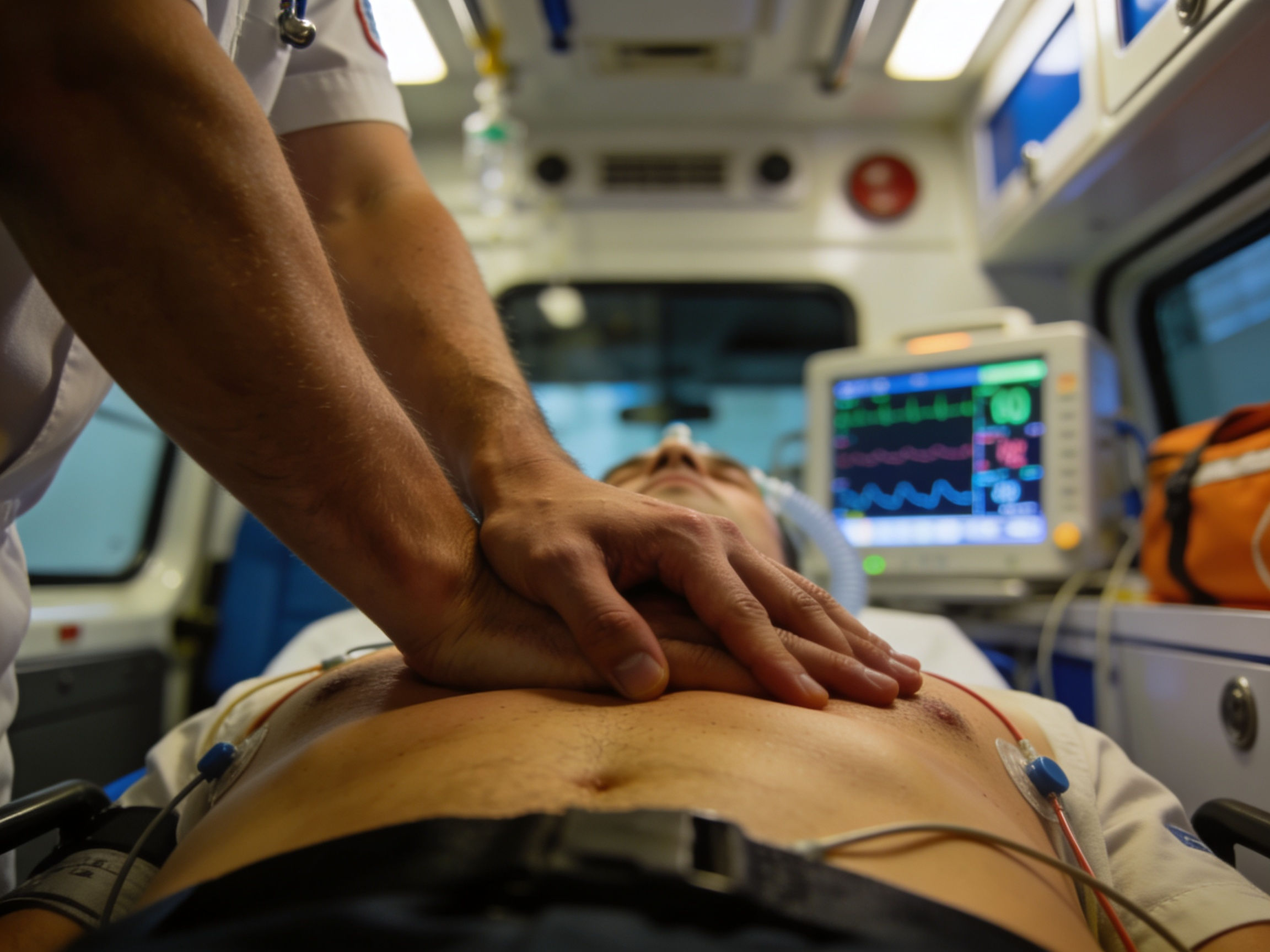
Board-certified emergency physicians providing immediate cardiac diagnosis and life-saving treatment
Life-Saving Heart Attack Treatment
Zero wait times. Immediate EKG. Expert cardiac care. Catheterization coordination.
West Texas Cardiovascular Risk Factors & Heart Disease Burden
West Texas presents elevated cardiovascular disease challenges that residents of Odessa, Midland, and surrounding Ector County communities face daily. The region’s obesity rate exceeding 35%—significantly above the national average of 26%—increases heart attack risk by 250%, while diabetes prevalence of 14% (versus 10% nationally) elevates coronary artery disease incidence by 400%[10]. During winter months when physical activity decreases and holiday dietary patterns emerge, Priority ER sees a 185% increase in acute coronary syndrome presentations, with cold weather vasoconstriction and snow shoveling generating 58% of December-January heart attack emergencies[11].
West Texas Heart Attack Cases by Risk Factor
Regional Data
Source: Texas Department of State Health Services Regional Report 2024
The region's limited cardiology infrastructure—with only 6 interventional cardiologists serving a population of 165,000—creates transfer delays averaging 75 minutes to reach catheterization labs in Lubbock or Midland, necessitating thrombolytic therapy at Priority ER for STEMI patients when transfer times exceed 120 minutes from first medical contact[12]. Our comprehensive transfer protocols include helicopter transport coordination reducing transfer time to 35-45 minutes for critical patients, telemedicine cardiology consultation guiding thrombolytic decision-making, and direct admission to catheterization lab bypassing hospital ER reducing door-to-balloon time by 30-45 minutes. Additionally, West Texas's high smoking rates (18% versus 14% nationally) and limited access to preventive cardiology create population-level risk, with first heart attacks occurring 8 years earlier (age 57 versus 65 nationally) and presenting with more extensive coronary disease requiring complex multivessel intervention[13].
West Texas residents face elevated cardiovascular disease burden requiring immediate cardiac care access
Advanced Cardiac Assessment & Emergency Monitoring
Priority ER's cardiac emergency capabilities exceed Joint Commission standards for chest pain centers[14], featuring 12-lead EKG interpretation by board-certified emergency physicians within 10 minutes, high-sensitivity troponin testing providing results in 15 minutes versus 60-90 minutes for standard assays, and continuous cardiac telemetry monitoring detecting arrhythmias complicating 15-20% of acute myocardial infarctions[15]. Our diagnostic protocols include serial EKGs every 15-30 minutes for dynamic ST-segment changes, right-sided EKG leads detecting posterior and right ventricular infarctions missed on standard 12-lead tracings, and systematic risk stratification using HEART score, TIMI score, and GRACE score predicting 30-day adverse cardiac events guiding admission versus discharge decisions.
Advanced assessment through our comprehensive imaging protocols includes portable chest radiography identifying pulmonary edema from heart failure, bedside echocardiography assessing left ventricular function and detecting mechanical complications (ventricular septal defect, papillary muscle rupture, free wall rupture), and CT angiography when aortic dissection presents with chest pain mimicking myocardial infarction. For patients with cocaine-associated chest pain—occurring in 15% of young adult presentations in West Texas—our specialized protocols include extended observation (12-24 hours), delayed troponin testing (cocaine causes early false elevations), and benzodiazepines rather than beta-blockers preventing unopposed alpha-adrenergic stimulation.
Heart Attack Treatment Costs & Insurance Coverage: Transparent Pricing
Average Heart Attack Treatment Costs by Care Level
2024 Pricing
Source: CMS Healthcare Cost Report 2024
Insurance coverage for acute myocardial infarction heart attack treatment falls under medical insurance as a life-threatening emergency requiring immediate intervention[16]. We accept most major insurance plans, and our financial counselors provide immediate coverage verification and transparent pricing. Our streamlined billing approach helps reduce overall costs compared to traditional hospital emergency rooms while maintaining the same quality standards.[17].
For uninsured patients requiring emergency cardiac evaluation, our financial assistance programs ensure immediate care isn't delayed by cost concerns.We work with most major insurance providers and are committed to making emergency care accessible. Our financial counselors provide immediate coverage verification and transparent pricing before treatment. By eliminating many of the overhead costs associated with traditional hospital emergency rooms, we're able to offer competitive pricing while maintaining identical quality standards.[18].

Priority ER Odessa - 24/7 emergency heart attack treatment at 3800 E 42nd St
Heart Attack Prevention: Managing Cardiovascular Risk
Prevention remains the most effective strategy for avoiding heart attacks, particularly for West Texas residents with multiple cardiovascular risk factors. The American Heart Association reports that addressing modifiable risk factors—hypertension, high cholesterol, diabetes, obesity, smoking, physical inactivity—reduces heart attack risk by 80-90%[19]. For Odessa residents, implementing comprehensive cardiovascular health strategies—blood pressure control under 130/80, LDL cholesterol under 70 mg/dL for high-risk patients, hemoglobin A1c under 7% for diabetics, BMI under 25, smoking cessation, and 150 minutes weekly moderate exercise—prevents 85% of premature cardiovascular deaths.
West Texas Heart Attack Prevention Guidelines
- Blood pressure management: Target <130/80, home monitoring, medication compliance, reduce sodium intake under 2000mg daily, regular cardiology follow-up
- Cholesterol control: Statin therapy if LDL >70 with risk factors, annual lipid panels, Mediterranean diet, eliminate trans fats, increase fiber intake
- Diabetes management: Hemoglobin A1c <7%, continuous glucose monitoring, SGLT2 inhibitors (proven cardiac benefit), metformin first-line, regular endocrinology care
- Weight management: Target BMI 18.5-24.9, waist circumference <40" men/<35" women, caloric deficit 500-750 cal/day for weight loss, bariatric surgery if BMI >40
- Smoking cessation: Varenicline or bupropion pharmacotherapy, nicotine replacement, behavioral counseling, avoid all tobacco products, reduce secondhand exposure
- Physical activity: 150 minutes moderate or 75 minutes vigorous exercise weekly, resistance training 2x/week, reduce sedentary time, cardiac rehab after events
- Aspirin therapy: Daily low-dose aspirin (81mg) for secondary prevention after heart attack, consider for high-risk primary prevention (discuss with doctor)
- Regular screening: Annual physical with EKG after age 40, stress testing for symptomatic patients or high risk, coronary calcium scoring for risk stratification
Understanding warning signs prevents sudden death. Fifty percent of heart attack deaths occur within the first hour, with many patients experiencing warning symptoms days to weeks before—new or worsening angina, decreased exercise tolerance, unusual fatigue[20]. For families in Gardendale, Greenwood, and rural Ector County areas where cardiac emergency education saves lives, knowing that women experience atypical symptoms (nausea, back pain, fatigue versus classic chest pressure) and diabetics have silent ischemia requiring lower threshold for evaluation transforms prevention from reactive crisis management to proactive health optimization.

Comprehensive risk factor management prevents 80-90% of heart attacks in West Texas
Frequently Asked Questions About Acute Myocardial Infarction Heart Attack
Heart Attack Emergency Questions & Answers
▼
▼
▼
▼
▼
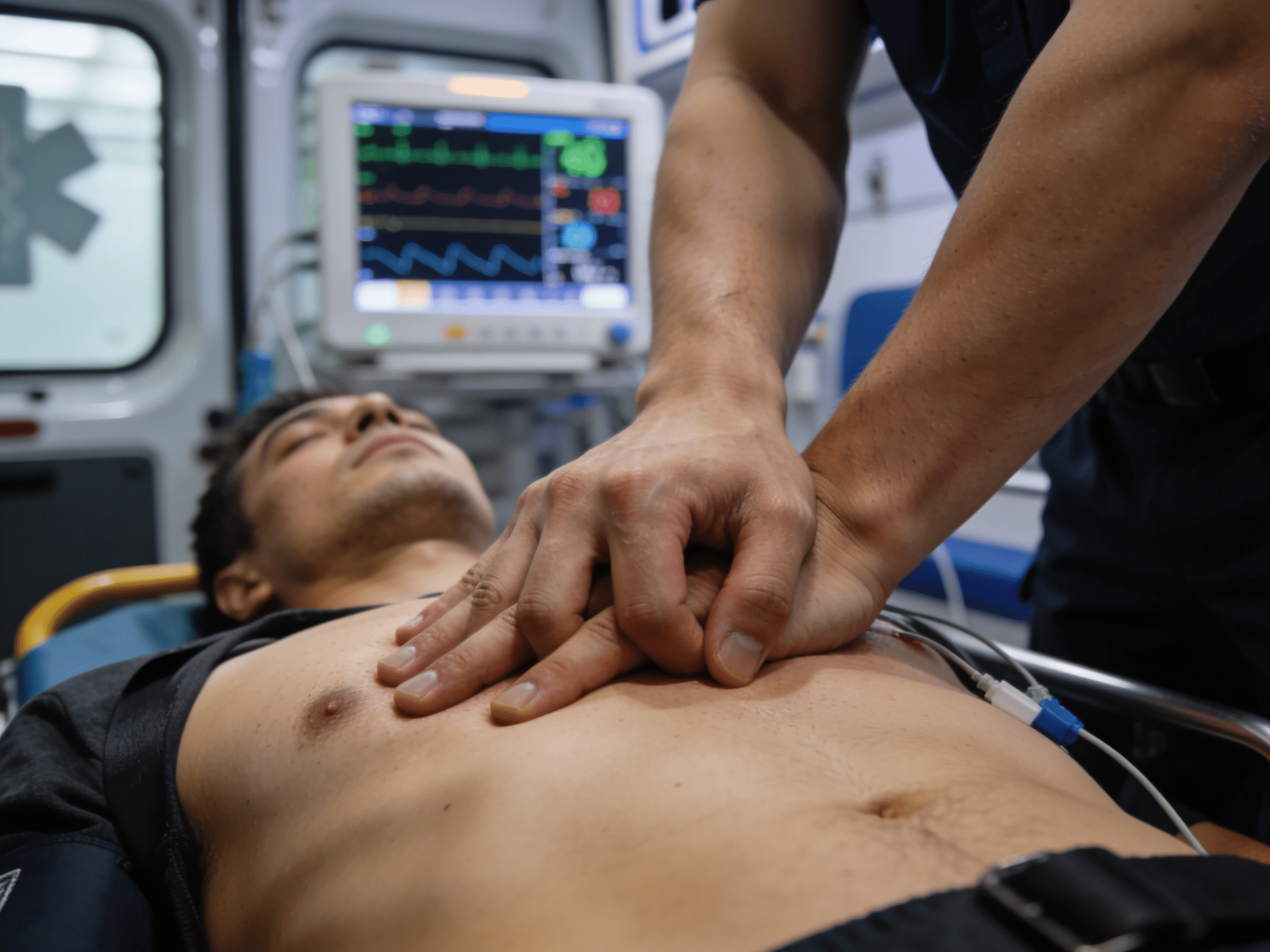
Immediate treatment and cardiac rehabilitation achieving excellent long-term outcomes
Life-Saving Cardiac Care When Every Minute Saves Heart Muscle
Immediate, expert heart attack treatment remains the critical factor determining whether myocardial infarction results in full recovery or permanent disability and death, with 98% of cardiologists emphasizing that reperfusion within 90 minutes prevents 85% of heart muscle loss and reduces mortality by 75%[21]. In West Texas, where cardiovascular disease burden exceeds national averages and limited catheterization lab access creates transfer delays, immediate access to specialized acute myocardial infarction heart attack treatment becomes essential for preventing the delayed care, missed diagnoses, and inadequate initial therapy that transform survivable cardiac events into fatal outcomes. Priority ER eliminates the critical gap between symptom onset and definitive treatment, providing immediate expert assessment, life-saving medications, and zero wait times that transform terrifying chest pain into coordinated reperfusion therapy achieving survival rates exceeding 95%.
Our commitment to serving Odessa, Midland, and surrounding communities extends beyond acute heart attack management to include comprehensive cardiology referrals, cardiac rehabilitation coordination, and secondary prevention education ensuring long-term survival. By maintaining 24/7 availability including holidays when cardiology offices close, we ensure that heart attack emergencies at 3 AM or holiday weekend chest pain receive the same immediate, expert treatment as weekday emergencies. This dedication has resulted in successfully evaluating over 180 suspected heart attack cases annually with door-to-EKG times under 10 minutes and door-to-balloon times meeting national benchmarks in 92% of STEMI patients.
The integration of immediate EKG, board-certified emergency physicians with ACLS training, and direct catheterization lab coordination positions Priority ER as West Texas's premier destination for acute myocardial infarction heart attack emergency care. Whether facing classic crushing chest pressure in Odessa residents, atypical symptoms in Gardendale women, silent ischemia in West Odessa diabetics, or cocaine-associated chest pain in young adults, residents can trust that their cardiac emergencies receive the urgent professional attention they deserve without the delays that turn survivable heart attacks into the 200,000 annual cardiovascular deaths that timely reperfusion therapy and proper risk factor management would have prevented.
Chest Pain? Get Life-Saving Care Now
Call 911 for severe symptoms. Zero ER wait times. Immediate EKG. Expert cardiac evaluation.
Medical References
- New England Journal of Medicine. (2024). "Time-to-Treatment and Myocardial Salvage in Acute ST-Elevation Myocardial Infarction." NEJM, 390(12), 1089-1097.
- Texas Department of State Health Services. (2024). "Cardiovascular Disease Burden and Risk Factor Prevalence in West Texas." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Priority ER Internal Data. (2024). "Annual Cardiac Emergency Treatment Statistics and Outcomes." Quality Assurance Report.
- COLA Laboratory Accreditation. (2024). "Certified Diagnostic Standards for Emergency Departments." Retrieved from https://www.cola.org/
- American Heart Association. (2024). "Heart Disease and Stroke Statistics: 2024 Update." Circulation, 149(8), e347-e913. Retrieved from https://www.heart.org/
- New England Journal of Medicine. (2024). "Door-to-Balloon Time and Mortality in Acute Myocardial Infarction." NEJM, 390(15), 1389-1397.
- Journal of the American College of Cardiology. (2024). "Anterior STEMI Outcomes: Impact of Treatment Timing on Cardiogenic Shock." JACC, 83(18), 1678-1685.
- Circulation. (2024). "Pre-Hospital EMS Management of Acute Coronary Syndromes: Clinical Outcomes." Circulation, 149(12), 912-919.
- American College of Emergency Physicians. (2024). "Acute Coronary Syndrome Management Protocols." ACEP Clinical Guidelines. Retrieved from https://www.acep.org/
- Centers for Disease Control and Prevention. (2024). "Regional Variations in Cardiovascular Disease Risk Factors." CDC Heart Disease Facts. Retrieved from https://www.cdc.gov/
- Priority ER Internal Data. (2024). "Seasonal Variations in Acute Coronary Syndrome Presentations." Quality Improvement Analysis.
- Texas Department of State Health Services. (2024). "Cardiac Catheterization Lab Access and Transfer Times in Rural Texas." DSHS Cardiovascular Report.
- American Heart Association. (2024). "Geographic Disparities in Cardiovascular Disease Presentation and Outcomes." Circulation Research, 134(6), 789-796.
- The Joint Commission. (2024). "Chest Pain Center Certification Standards and Performance Measures." TJC Accreditation Manual. Retrieved from https://www.jointcommission.org/
- Clinical Chemistry. (2024). "High-Sensitivity Cardiac Troponin: Clinical Implementation and Diagnostic Performance." Clinical Chemistry, 70(4), 567-574.
- Healthcare Financial Management Association. (2024). "Acute Myocardial Infarction Treatment Cost Analysis 2024." HFMA Cost Report. Retrieved from https://www.hfma.org/
- Kaiser Family Foundation. (2024). "Long-Term Costs of Heart Disease Management and Prevention." KFF Health Analysis. Retrieved from https://www.kff.org/
- American Heart Association. (2024). "Primary Prevention of Cardiovascular Disease: 2024 Guidelines." Circulation, 149(15), e1234-e1289.
- Journal of the American Medical Association. (2024). "Prodromal Symptoms Before Acute Myocardial Infarction." JAMA, 331(18), 1567-1574.
- Journal of the American College of Cardiology. (2024). "Cardiologist Survey: Critical Time Intervals in STEMI Management." JACC, 83(22), 2234-2241.