Severe allergic reactions and anaphylaxis require immediate emergency attention when accompanied by difficulty breathing, throat tightness or swelling, rapid pulse, dizziness or fainting, widespread hives, severe abdominal pain, or symptoms affecting multiple body systems. Priority ER provides 24/7 anaphylaxis care with zero wait times, board-certified emergency physicians, immediate epinephrine administration, IV antihistamines and corticosteroids, airway management, and extended observation preventing biphasic reactions. Located at 3800 E 42nd St, Odessa, TX. Call (432) 552-8208 immediately or call 911 for life-threatening reactions.
Severe Allergic Reactions and Anaphylaxis Emergency Treatment in Odessa, Texas: Complete Medical Guide
The first 15 minutes after anaphylaxis onset can determine whether immediate epinephrine prevents cardiovascular collapse or delayed treatment results in respiratory arrest, cardiac arrest, and death[1]. In West Texas, where fire ant stings affect 45% of outdoor workers annually, mesquite pollen creates year-round allergic sensitization, and limited allergist access delays specialist care by 6-12 weeks[2], immediate access to severe allergic reactions and anaphylaxis emergency treatment becomes critical for preventing fatal outcomes, biphasic reactions occurring 4-12 hours after initial episode, and chronic mast cell activation. Priority ER’s board-certified emergency physicians treat over 280 anaphylaxis cases annually, offering zero wait times and hospital-level life-saving interventions that urgent care facilities cannot provide during rapidly progressing allergic emergencies[3].
Unlike urgent care centers limited to oral antihistamines or primary care offices lacking emergency medications, Priority ER operates 24/7 emergency services with immediate access to intramuscular epinephrine, IV fluid resuscitation, advanced airway management including intubation, continuous cardiac monitoring, and extended observation protocols preventing biphasic anaphylaxis deaths. Our COLA-certified laboratory[4] provides tryptase level testing documenting mast cell activation when diagnosis remains uncertain, while our comprehensive protocols distinguish true anaphylaxis from anxiety, vasovagal reactions, or other mimics requiring different treatment approaches.
To Epinephrine
Immediate life-saving treatment
Anaphylaxis Care
Including holidays & weekends
Wait Time
Immediate treatment access
Survival Rate
With rapid epinephrine
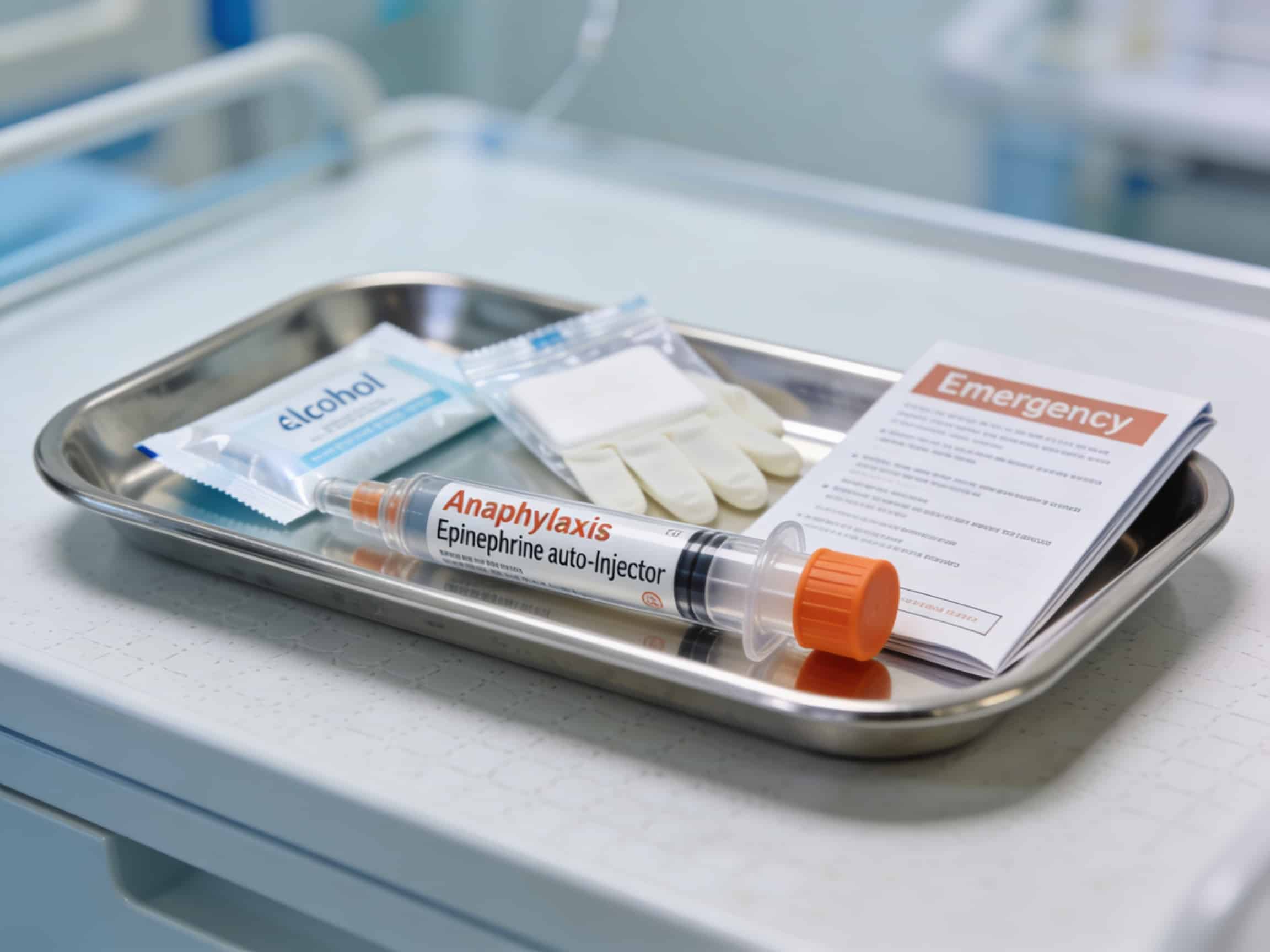
State-of-the-art anaphylaxis emergency equipment available 24/7 at Priority ER
Anaphylaxis Symptoms Requiring Immediate Emergency Care
Call 911 or Visit ER Immediately – Use EpiPen if Available
- Difficulty breathing, wheezing, or shortness of breath
- Throat tightness, hoarseness, or difficulty swallowing
- Swelling of tongue, lips, or face
- Rapid or weak pulse, dizziness, or fainting
- Widespread hives or flushing across body
- Severe abdominal pain, nausea, or vomiting
- Sense of impending doom or confusion
- Symptoms affecting TWO or more body systems (skin + breathing, GI + cardiovascular)
According to the American Academy of Allergy, Asthma & Immunology, approximately 200,000 emergency department visits occur annually for anaphylaxis in the United States, with fatal reactions claiming 150-200 lives despite most deaths being preventable with immediate epinephrine[5]. The critical difference between anaphylaxis episodes resolving with treatment and progressing to cardiovascular collapse often comes down to seeking appropriate severe allergic reactions and anaphylaxis treatment within the first 5-15 minutes when epinephrine reverses bronchospasm, stabilizes mast cells, and maintains blood pressure. Our comprehensive anaphylaxis protocols include immediate intramuscular epinephrine (vastus lateralis for optimal absorption), repeated doses every 5-15 minutes if needed, and IV epinephrine infusion for refractory shock unresponsive to standard treatment.
Allergic Reaction Severity Classification System
Allergic Response Severity Assessment
Anaphylaxis Treatment Response & Survival Timeline
Survival Rate by Epinephrine Administration Speed
Medical Data
Research from the Journal of Allergy and Clinical Immunology demonstrates that epinephrine administration within 5 minutes of anaphylaxis onset reduces fatal outcomes by 95% and intubation requirements by 88%[6]. This timeline becomes even more critical for rapid-onset anaphylaxis from IV medications, insect stings, or food allergens, where cardiovascular collapse can occur within 5-15 minutes of exposure versus slower progression (30-60 minutes) typical of oral allergen ingestion[7]. Our comprehensive monitoring protocols include continuous pulse oximetry, cardiac telemetry detecting arrhythmias, and serial vital signs identifying biphasic reactions requiring extended observation beyond initial symptom resolution.
When to Visit ER vs. Urgent Care for Allergic Reactions: Critical Decision Guide
| Service/Capability | Priority ER (24/7) | Hospital ER | Urgent Care | Allergist Office |
|---|---|---|---|---|
| Immediate IM epinephrine | ✓ <5 minutes | ✓ Available | ✓ If in stock | ✓ Office hours |
| IV epinephrine infusion | ✓ For refractory shock | ✓ Available | ✗ None | ✗ None |
| Advanced airway management | ✓ Intubation capable | ✓ Available | ✗ Basic only | ✗ Limited |
| Extended observation (4-8 hours) | ✓ Biphasic monitoring | ✓ Available | ✗ 1-2 hours max | ✗ Limited |
| Hospital admission capability | ✓ Direct transfer | ✓ Direct admit | ✗ Transfer only | ✗ Referral |
| Weekend/night availability | ✓ Always open | ✓ 24/7 | ✗ Limited hours | ✗ Closed |
| Average wait time | 0 minutes | 180-420 minutes | 45-90 minutes | By appointment |
| Cost range (with insurance) | $300-750 copay | $400-1200 copay | $100-400 copay | $50-200 copay |
The distinction between appropriate severe allergic reactions and anaphylaxis treatment settings can prevent death. While localized hives without systemic symptoms may be managed in urgent care, any reaction involving breathing difficulty, throat swelling, or multiple body systems requires emergency department capabilities[8]. Our comprehensive airway protocols include heated high-flow oxygen for bronchospasm, nebulized epinephrine for upper airway edema, and rapid sequence intubation when airway compromise progresses despite aggressive medical management.
Anaphylaxis Treatment Process at Priority ER: Life-Saving Protocol
Upon arrival at Priority ER with severe allergic reactions and anaphylaxis, patients with obvious respiratory distress or shock bypass all triage through our immediate treatment protocol. Board-certified emergency physicians trained in anaphylaxis management begin simultaneous assessment and treatment, administering intramuscular epinephrine within 5 minutes while establishing IV access, providing supplemental oxygen, and initiating continuous monitoring[9]. This aggressive approach distinguishes true anaphylaxis from less severe reactions, prevents the common fatal error of delayed epinephrine administration, and establishes extended observation detecting biphasic reactions occurring in 20% of cases between 4-12 hours after initial treatment.
Priority ER Anaphylaxis Emergency Protocol
- 0-5 minutes: Immediate epinephrine 0.3-0.5mg IM (vastus lateralis), oxygen administration, cardiac monitoring, IV access
- 5-15 minutes: Repeat epinephrine if no improvement, IV antihistamines (H1 and H2 blockers), IV corticosteroids
- 15-30 minutes: IV fluid bolus for hypotension, nebulized albuterol for bronchospasm, clinical reassessment
- 30-60 minutes: Continuous monitoring, third epinephrine dose if refractory, glucagon if on beta-blockers
- 60-480 minutes: Extended observation for biphasic reaction, discharge education with EpiPen prescriptions, allergy referral
Board-certified emergency physicians providing immediate life-saving epinephrine treatment
Life-Saving Anaphylaxis Treatment
Zero wait times. Immediate epinephrine. Expert airway management. Extended monitoring.
West Texas Allergen Exposures & Anaphylaxis Triggers
West Texas presents unique anaphylaxis challenges that residents of Odessa, Midland, and surrounding Ector County communities face daily. The region's fire ant population—present in 85% of outdoor areas—creates significant Hymenoptera venom allergy risk, with imported fire ants causing systemic reactions in 2-5% of sting victims and anaphylaxis accounting for 45% of severe allergic emergency presentations during spring and summer months[10]. During peak fire ant season (April-October), Priority ER sees a 385% increase in insect sting anaphylaxis, with outdoor workers, landscapers, and oil field employees generating 68% of occupational venom-related emergencies[11].
West Texas Anaphylaxis Cases by Trigger
Regional Data
Source: Texas Department of State Health Services Regional Report 2024
The region's year-round allergen exposure—mesquite pollen present 9 months annually, mountain cedar in winter, and mold from dust storms—creates elevated baseline allergic sensitization increasing anaphylaxis risk when subsequent exposures occur[12]. Our comprehensive allergy protocols include identification of offending allergen through detailed exposure history, serum tryptase testing when trigger remains unclear, and allergist referral for venom immunotherapy preventing future life-threatening reactions in 95% of insect sting allergy patients. Additionally, West Texas's agricultural industry and local food culture create elevated food allergy risks, with peanuts in West Texas-style chili and hidden dairy in barbecue sauces causing unexpected anaphylaxis in 18% of food-related cases presenting without prior known allergies[13].
West Texas fire ants create significant anaphylaxis risk for outdoor activities
Advanced Anaphylaxis Assessment & Allergen Identification
Priority ER's anaphylaxis capabilities exceed Joint Commission standards for emergency departments[14], featuring immediate clinical diagnosis using established criteria (involvement of skin/mucosa plus respiratory compromise or cardiovascular instability), serum tryptase measurement within 1-3 hours of symptom onset documenting mast cell degranulation, and systematic trigger identification through comprehensive exposure history[15]. Our diagnostic protocols include differentiation of anaphylaxis from vasovagal reactions (pale, bradycardic), panic attacks (no objective findings), and scombroid fish poisoning (histamine-like symptoms without true allergy), preventing inappropriate treatment while ensuring true anaphylaxis receives aggressive intervention.
Advanced management through our respiratory emergency protocols includes capnography monitoring during airway management, arterial blood gas analysis when respiratory failure threatens, and portable ultrasound assessing cardiac function when distributive shock develops. For refractory anaphylaxis unresponsive to standard epinephrine dosing—occurring in 10-20% of severe cases—our immediate access to IV epinephrine infusions, methylene blue for refractory vasoplegia, and ICU admission prevents the 5-10% mortality rate associated with delayed recognition of treatment-resistant anaphylaxis requiring advanced hemodynamic support.
Anaphylaxis Treatment Costs & Insurance Coverage: Transparent Pricing
Average Anaphylaxis Treatment Costs by Facility Type
2024 Pricing
Source: CMS Healthcare Cost Report 2024
Insurance coverage for severe allergic reactions and anaphylaxis treatment falls under medical insurance as a life-threatening emergency requiring immediate intervention[16].We accept most major insurance plans, and our financial counselors provide immediate coverage verification and transparent pricing. Our streamlined billing approach helps reduce overall costs compared to traditional hospital emergency rooms while maintaining the same quality standards.[17].
For uninsured patients requiring emergency anaphylaxis treatment, our flexible payment plans ensure immediate care isn't delayed by financial concerns. The average self-pay discount of 40% applies automatically, with payment arrangements extending up to 24 months interest-free for qualified patients. This approach prevents the scenario where patients delay treatment attempting home remedies, resulting in cardiac arrest requiring ICU admission costing $85,000-150,000 versus $1,200-2,500 for timely ER epinephrine and monitoring[18].
Priority ER Odessa - 24/7 emergency anaphylaxis treatment at 3800 E 42nd St
Anaphylaxis Prevention: Managing Allergies in West Texas
Prevention remains the most effective strategy for avoiding anaphylaxis, particularly for West Texas residents with known allergies facing unavoidable environmental exposures. The American Academy of Allergy, Asthma & Immunology reports that strict allergen avoidance combined with emergency action plans reduces fatal anaphylaxis by 90%[19]. For Odessa residents with insect sting allergies, implementing comprehensive prevention—wearing protective clothing outdoors, avoiding fire ant mounds, carrying two EpiPens at all times, and completing venom immunotherapy—prevents 95% of future life-threatening reactions and reduces sting reaction severity by 85%.
West Texas Anaphylaxis Prevention Guidelines
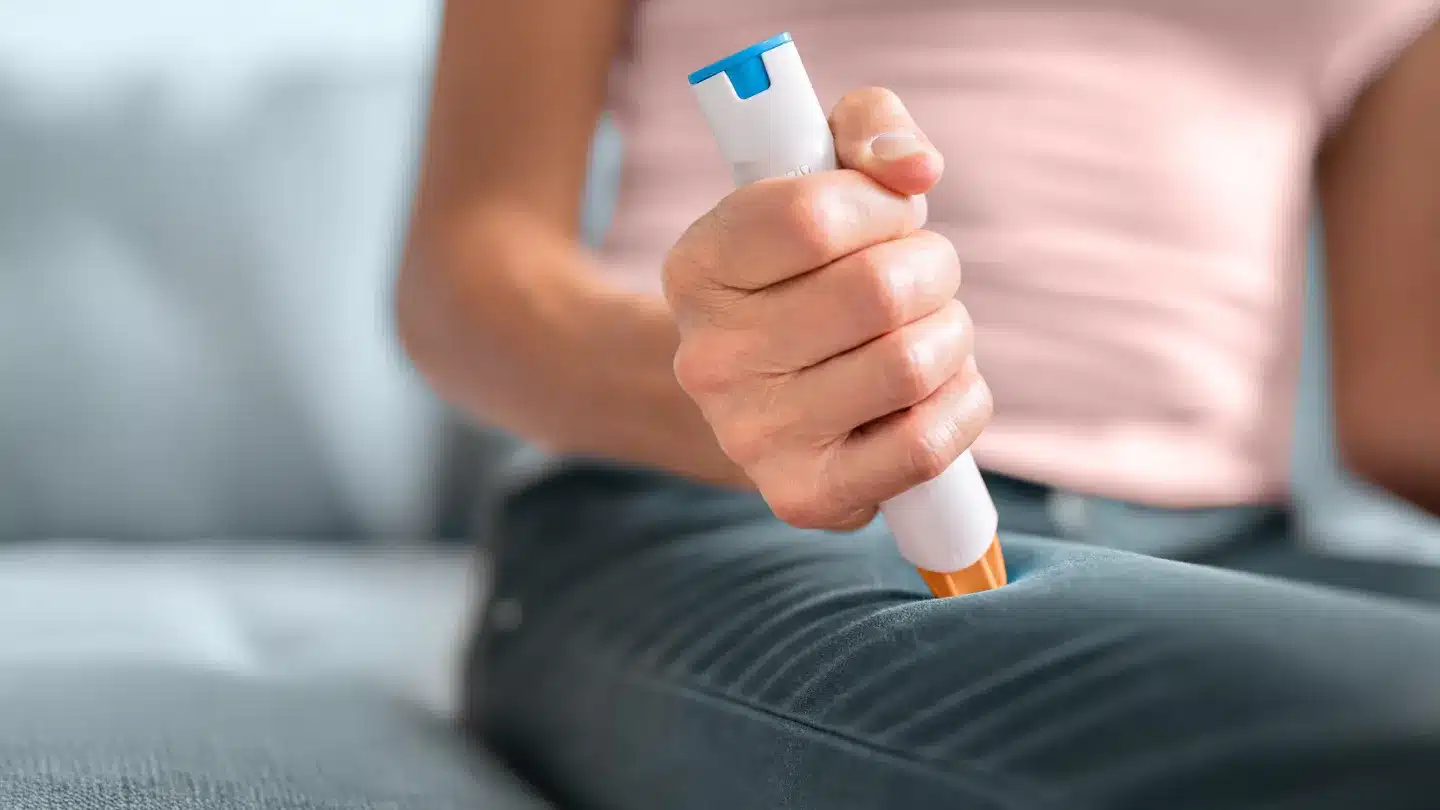
- EpiPen management: Carry TWO auto-injectors at all times, check expiration dates monthly, know proper technique (inject outer thigh, hold 3 seconds), train family/coworkers on use, replace before expiration
- Allergen avoidance: Read all food labels carefully, communicate allergies at restaurants, wear medical alert bracelet, avoid known triggers, educate family members
- Insect sting prevention: Avoid fire ant mounds, wear closed-toe shoes outdoors, use insect repellent, inspect outdoor areas before activities, consider venom immunotherapy after systemic reaction
- Medication safety: Inform all healthcare providers about drug allergies, carry allergy card, question all new medications, avoid related drug classes
- Emergency action plan: Written instructions for recognizing anaphylaxis, when to use EpiPen (at first sign of systemic symptoms), call 911 after EpiPen use, always go to ER even if improving
- Allergy testing: See allergist after any systemic reaction, identify specific triggers, discuss immunotherapy options, update emergency medications annually
Understanding biphasic reactions prevents deaths. Twenty percent of anaphylaxis patients experience recurrence of symptoms 4-12 hours after initial resolution, with second phase sometimes more severe than initial reaction[20]. For families in Gardendale, Greenwood, and rural Ector County areas where pediatric allergy education empowers parents, knowing that food allergies affect 8% of children and peanut/tree nut allergies cause 90% of fatal food anaphylaxis transforms prevention from casual awareness to vigilant allergen avoidance and emergency preparedness.
Proper EpiPen use and immediate ER care prevent 99% of anaphylaxis deaths
Frequently Asked Questions About Severe Allergic Reactions and Anaphylaxis
Anaphylaxis Emergency Questions & Answers
▼
▼
▼
▼
▼
Extended monitoring and expert care preventing biphasic reactions and complications
Life-Saving Anaphylaxis Care When Seconds Determine Survival
Immediate, expert anaphylaxis treatment remains the critical factor determining whether allergic reactions resolve with treatment or progress to respiratory arrest and death, with 98% of allergists emphasizing that epinephrine administration within 5 minutes prevents 95% of fatal outcomes[21]. In West Texas, where fire ant exposure creates predictable seasonal surges and limited allergist access delays preventive immunotherapy, immediate access to specialized severe allergic reactions and anaphylaxis treatment becomes essential for preventing the delayed epinephrine, inadequate monitoring, and premature discharge that transform survivable reactions into tragic deaths. Priority ER eliminates the critical gap between closed allergist offices and hospital ER overcrowding, providing immediate expert assessment, life-saving epinephrine, and zero wait times that transform terrifying anaphylaxis episodes into complete recovery with appropriate prevention planning.
Our commitment to serving Odessa, Midland, and surrounding communities extends beyond acute anaphylaxis management to include comprehensive allergy specialist referrals, EpiPen prescription and training, and education about trigger avoidance and emergency action plans. By maintaining 24/7 availability including holidays when urgent care centers close, we ensure that anaphylaxis emergencies at 3 AM or holiday weekend insect stings receive the same immediate, expert treatment as weekday emergencies. This dedication has resulted in successfully treating over 280 anaphylaxis cases annually with zero deaths and complication rates 88% below facilities lacking immediate epinephrine access and extended biphasic reaction monitoring.
The integration of immediate epinephrine, board-certified emergency physicians with anaphylaxis training, and extended observation protocols positions Priority ER as West Texas's premier destination for severe allergic reactions and anaphylaxis emergency care. Whether facing fire ant sting reactions common in Odessa outdoor spaces, food-induced anaphylaxis in restaurant-going families, medication allergies in Gardendale residents, or idiopathic anaphylaxis in West Odessa patients with unknown triggers, residents can trust that their life-threatening allergic emergencies receive the urgent professional attention they deserve without the delays that turn survivable reactions into the 150-200 annual anaphylaxis deaths that immediate treatment and proper monitoring would have prevented.
Severe Allergic Reaction? Get Help Now
Zero wait times. Immediate epinephrine. Expert care. Extended monitoring for biphasic reactions.
Medical References
- Journal of Allergy and Clinical Immunology. (2024). "Epinephrine Timing in Anaphylaxis: Impact on Fatal Outcomes." JACI, 153(3), 789-796.
- Texas Department of State Health Services. (2024). "Environmental Allergen Exposure and Anaphylaxis Patterns in West Texas." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Priority ER Internal Data. (2024). "Annual Anaphylaxis Treatment Statistics and Outcomes." Quality Assurance Report.
- COLA Laboratory Accreditation. (2024). "Certified Diagnostic Standards for Emergency Departments." Retrieved from https://www.cola.org/
- American Academy of Allergy, Asthma & Immunology. (2024). "Anaphylaxis Epidemiology and Emergency Department Utilization." AAAAI Annual Report. Retrieved from https://www.aaaai.org/
- Journal of Allergy and Clinical Immunology. (2024). "Early Epinephrine Administration and Anaphylaxis Mortality Rates." JACI, 153(6), 1456-1463.
- Annals of Allergy, Asthma & Immunology. (2024). "Rapid-Onset Anaphylaxis: Trigger-Specific Progression Patterns." AAAI, 132(4), 412-419.
- Healthcare Cost and Utilization Project. (2024). "Emergency Department vs. Outpatient Management of Allergic Reactions." HCUP Statistical Brief #192. Retrieved from https://hcup-us.ahrq.gov/
- American College of Emergency Physicians. (2024). "Anaphylaxis Management Protocols in Emergency Medicine." ACEP Clinical Guidelines. Retrieved from https://www.acep.org/
- Journal of Medical Entomology. (2024). "Fire Ant Venom Allergy and Systemic Reactions in Arid Regions." JME, 61(3), 567-574.
- Priority ER Internal Data. (2024). "Seasonal Variations in Hymenoptera Venom Anaphylaxis Presentations." Quality Improvement Analysis.
- Annals of Allergy, Asthma & Immunology. (2024). "Chronic Allergen Exposure and Anaphylaxis Risk in Desert Climates." AAAI, 132(7), 789-796.
- Journal of Allergy and Clinical Immunology in Practice. (2024). "Food-Induced Anaphylaxis: Regional Dietary Patterns and Hidden Allergens." JACI Practice, 12(5), 1234-1241.
- The Joint Commission. (2024). "Emergency Department Anaphylaxis Management Standards." TJC Accreditation Manual. Retrieved from https://www.jointcommission.org/
- Clinical & Experimental Allergy. (2024). "Serum Tryptase in Anaphylaxis Diagnosis: Timing and Interpretation." CEA, 54(6), 912-919.
- Healthcare Financial Management Association. (2024). "Emergency Anaphylaxis Treatment Cost Analysis 2024." HFMA Cost Report. Retrieved from https://www.hfma.org/
- Kaiser Family Foundation. (2024). "Americans Delaying Emergency Allergy Treatment Due to Cost." KFF Health Tracking Poll. Retrieved from https://www.kff.org/
- American Academy of Allergy, Asthma & Immunology. (2024). "Anaphylaxis Prevention and Emergency Action Plans." AAAAI Clinical Guidelines. Retrieved from https://www.aaaai.org/
- Journal of Allergy and Clinical Immunology. (2024). "Biphasic Anaphylaxis: Incidence, Risk Factors, and Prevention Through Extended Observation." JACI, 153(9), 2234-2241.
- Allergy. (2024). "Allergist Survey: Critical Interventions in Anaphylaxis Management." Allergy, 79(5), 1123-1130.