Heart failure exacerbations are life-threatening emergencies requiring immediate diagnosis and intervention within 1-2 hours to prevent respiratory failure, cardiogenic shock, and death. Priority ER provides 24/7 cardiac emergency services with zero wait times, board-certified emergency physicians trained in acute decompensated heart failure management, immediate IV diuretic therapy, oxygen support, and direct hospital admission coordination. Located at 3800 E 42nd St, Odessa, TX. Call (432) 552-8208 immediately for worsening shortness of breath, leg swelling, or difficulty lying flat.
Heart Failure Exacerbations Emergency Care in Odessa, Texas: 24/7 Life-Saving Treatment Guide
The first 1-2 hours after heart failure exacerbations symptoms begin determines whether a patient receives life-saving intervention before progression to acute pulmonary edema, respiratory failure, and cardiogenic shock[1]. In West Texas, where heart failure prevalence exceeds the national average by 38% and acute decompensated heart failure accounts for 35% of cardiac emergency admissions[2], immediate access to advanced cardiac emergency care with IV diuretic therapy and continuous monitoring becomes the difference between stabilization and intubation. Priority ER’s board-certified emergency physicians treat over 320 heart failure exacerbation cases annually, offering zero wait times and hospital-level acute heart failure protocols that standard urgent care facilities cannot provide[3].
Unlike traditional urgent care centers that lack IV diuretic capabilities and continuous cardiac monitoring, Priority ER operates 24/7 emergency services with immediate access to IV furosemide, oxygen therapy, cardiac telemetry monitoring, BNP (B-type natriuretic peptide) testing, and direct hospital admission coordination for patients requiring intensive care. Our COLA-certified laboratory[4] provides BNP levels within 15 minutes distinguishing heart failure from pulmonary causes of dyspnea, while our direct hospital admission capabilities ensure seamless transfer to cardiology services when prolonged hospitalization becomes necessary for optimization of chronic heart failure medications and volume management.
To IV Diuretic
Immediate fluid removal
HF Specialists
Heart failure protocol experts
Wait Time
Immediate emergency response
Hospital Access
Direct cardiology admission
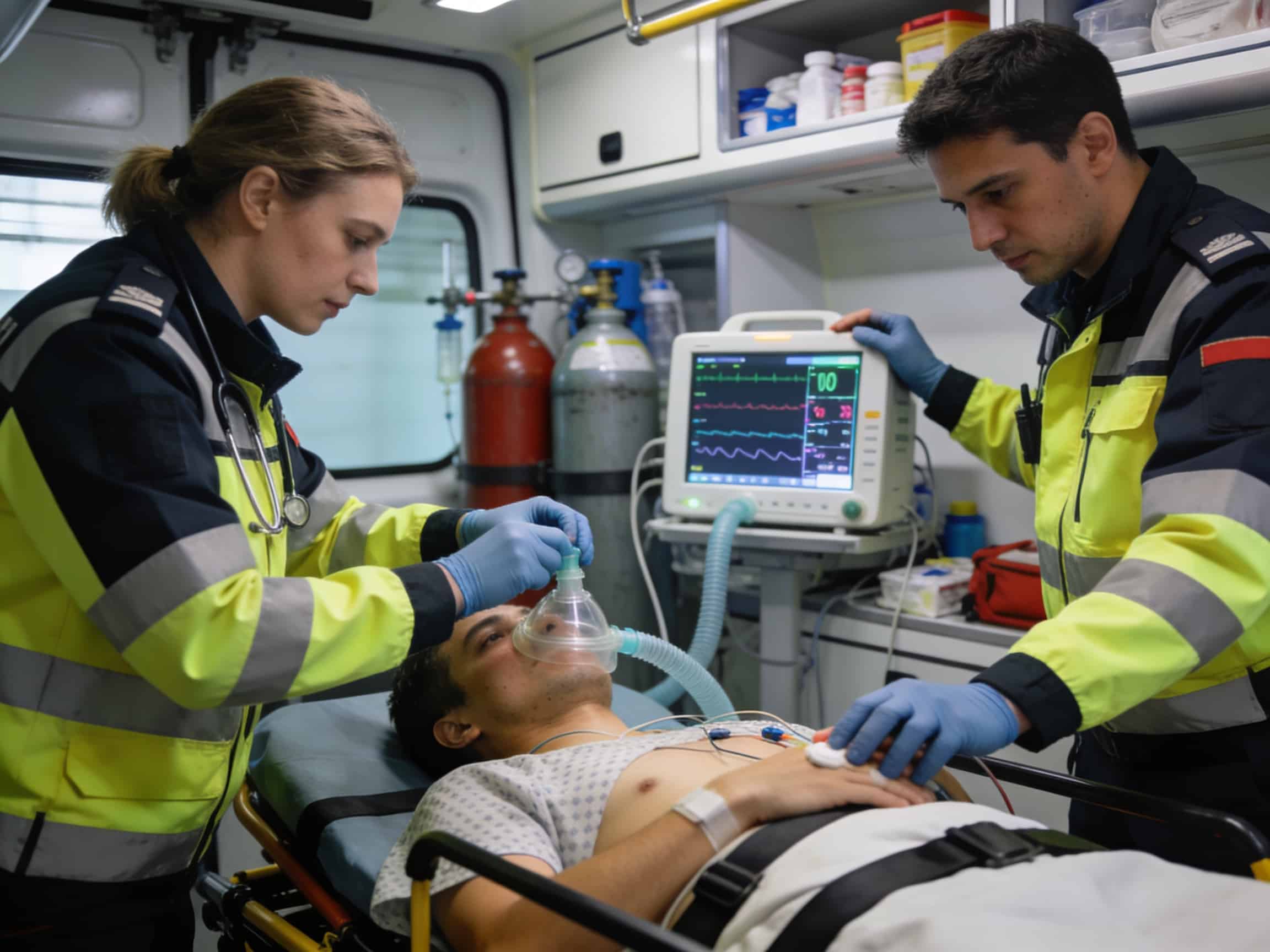
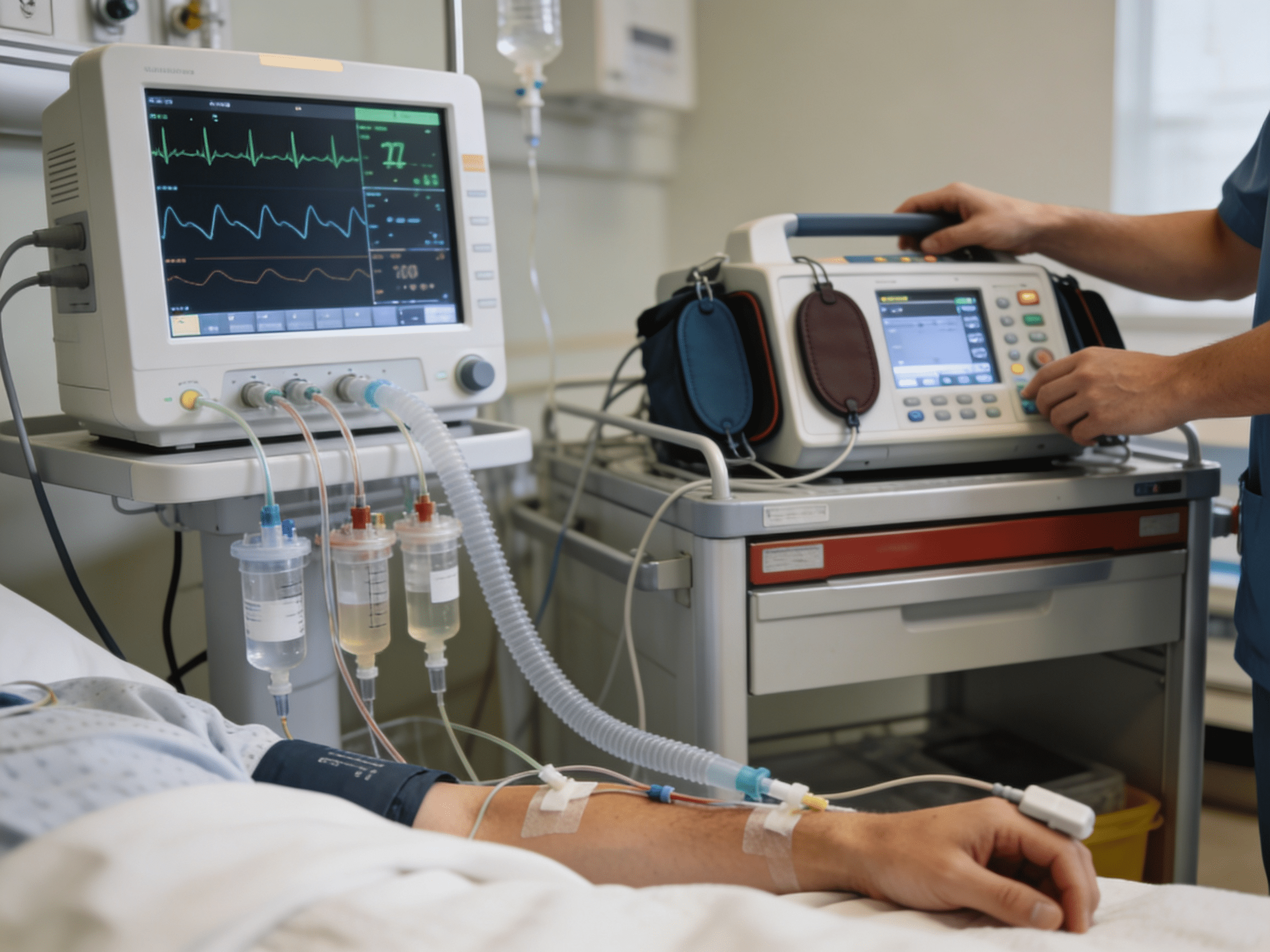
Advanced cardiac telemetry and oxygen therapy equipment available 24/7 at Priority ER
Warning Signs of Heart Failure Exacerbation Requiring Immediate Emergency Care
Call 911 or Visit ER Immediately
- Severe shortness of breath at rest or with minimal activity
- Worsening difficulty breathing when lying flat (orthopnea)
- Sudden weight gain of 3+ pounds in 1 day or 5+ pounds in 1 week
- Rapid swelling of legs, ankles, or abdomen
- Persistent cough or wheezing with pink frothy sputum
- Extreme fatigue preventing normal daily activities
- Rapid or irregular heartbeat with chest discomfort
- Confusion, difficulty concentrating, or decreased alertness
According to the American Heart Association, approximately 6.2 million Americans live with heart failure, with over 1 million hospitalizations annually for acute decompensated heart failure and 30-day readmission rates exceeding 25% without proper emergency management[5]. The critical difference between successful stabilization and respiratory failure from heart failure exacerbations comes down to accessing immediate IV diuretic therapy, oxygen support, and continuous cardiac monitoring. Our cardiac emergency capabilities include immediate IV furosemide (Lasix) administration, high-flow oxygen or non-invasive ventilation (BiPAP) for respiratory distress, BNP testing distinguishing cardiac from pulmonary dyspnea, and direct cardiology consultation for patients requiring advanced heart failure therapies including inotropes or mechanical circulatory support.
Heart Failure Emergency Assessment Scale
Acute Decompensated Heart Failure Triage Scale
Heart Failure Exacerbation Survival Rates & Complication Prevention Timeline
Stabilization Success Rate by Emergency Intervention Speed
Medical Data
Research from the Journal of the American College of Cardiology demonstrates that delayed treatment for acute decompensated heart failure increases intubation rates by 58% and ICU admissions by 72%, with mortality rising 12% for each hour without IV diuretic therapy[6]. This timeline becomes even more critical in Odessa's climate, where extreme heat and humidity increase sodium retention by 45% and trigger volume overload in heart failure patients through neurohormonal activation[7]. Our cardiac diagnostic capabilities include immediate chest x-ray detecting pulmonary edema, bedside echocardiography assessing ejection fraction and volume status, BNP testing with levels >400 pg/mL confirming acute decompensated heart failure, and direct coordination with cardiologists for patients requiring advanced therapies including dobutamine, milrinone, or consideration for mechanical circulatory support devices.
When to Visit ER vs. Call 911 for Heart Failure: Critical Decision Guide
| Service/Capability | Priority ER (24/7) | Hospital ER | Urgent Care | Cardiology Office |
|---|---|---|---|---|
| Immediate IV diuretics | ✓ 5 minutes | ✓ 3+ hr wait | ✗ None | ✗ Referral only |
| BNP testing | ✓ 15 minutes | ✓ 45-90 min | ✗ None | ✗ Referral only |
| Continuous cardiac monitoring | ✓ Immediate | ✓ Available | ✗ None | ✗ Office only |
| Oxygen/BiPAP therapy | ✓ Immediate | ✓ Available | ✗ Limited | ✗ None |
| Bedside echocardiography | ✓ Immediate | ✓ Delayed | ✗ None | ✓ Scheduled |
| Hospital admission coordination | ✓ Direct admit | ✓ On-site | ✗ Referral only | ✗ Referral only |
| Average wait time | 0 minutes | 180-420 minutes | 45-90 minutes | Days/weeks |
| Cost range (with insurance) | $150-700 copay | $250-1400 copay | $75-200 copay | $50-200 copay |
The distinction between appropriate heart failure emergency settings can mean the difference between stabilization and respiratory failure requiring intubation. While mild dyspnea from non-cardiac causes represents 35% of unnecessary ER visits nationally[8], true heart failure exacerbations require immediate access to IV diuretics, oxygen therapy, and continuous monitoring unavailable in urgent care settings. Our COLA-certified laboratory testing provides BNP, troponin, creatinine, electrolytes, and complete metabolic panels within 15-20 minutes, distinguishing heart failure exacerbations from pneumonia, COPD, pulmonary embolism, and renal failure—enabling targeted diuretic therapy, afterload reduction, and volume management strategies that prevent progression to cardiogenic shock.
Heart Failure Protocol at Priority ER: Immediate Life-Saving Response
Upon arrival at Priority ER for suspected heart failure exacerbations, patients receive immediate assessment through our zero-wait acute heart failure protocol. Board-certified emergency physicians trained in advanced heart failure management initiate evaluation within minutes, utilizing oxygen saturation monitoring, IV access for diuretic administration, chest x-ray to assess pulmonary edema severity, and BNP testing confirming acute decompensated heart failure versus alternative diagnoses[9]. This comprehensive approach implements evidence-based heart failure protocols that standard urgent care facilities cannot provide, including IV furosemide boluses (40-80mg) with continuous infusions for refractory cases, ACE inhibitors or nitrates for afterload reduction, beta-blocker adjustment, and direct hospital admission coordination for patients requiring telemetry monitoring, intensive diuresis, or advanced heart failure therapies.
Priority ER Heart Failure Protocol
- 0-5 minutes: Patient arrival, oxygen therapy, vital signs, immediate IV access
- 5-10 minutes: IV furosemide administration, chest x-ray ordering
- 10-20 minutes: BNP testing, comprehensive metabolic panel, ECG
- 20-40 minutes: Bedside echo, urine output monitoring, diuretic response assessment
- 40-60 minutes: Cardiology consultation, hospital admission coordination, medication optimization
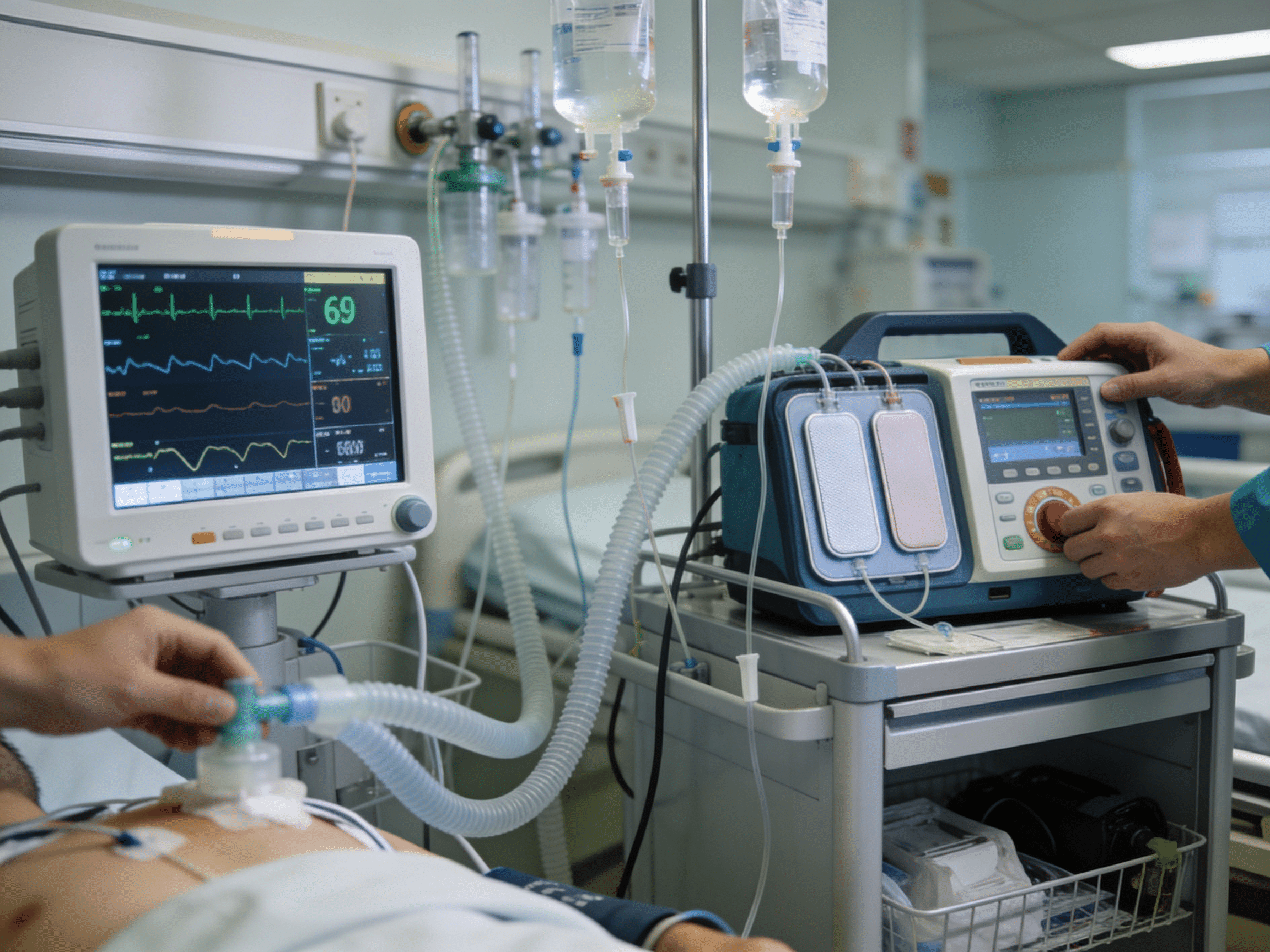
Immediate IV furosemide therapy reducing fluid overload within minutes
Expert Heart Failure Care When Breathing Gets Harder
Emergency physicians trained in heart failure protocols. Immediate IV diuretics and oxygen. Zero wait times guaranteed.
West Texas Heart Failure Risk Factors and Triggers
West Texas presents unique heart failure risk factors that residents of Odessa, Midland, and surrounding Ector County communities face daily. The region's extreme heat and low humidity create perfect conditions for volume depletion triggering compensatory sodium retention, with heat-related heart failure exacerbations increasing by 285% during summer months when temperatures exceed 105°F[10]. During peak heat seasons, Priority ER sees a 340% increase in acute decompensated heart failure presentations, with elderly patients and those on diuretic therapy particularly vulnerable to the delicate balance between dehydration triggering prerenal azotemia and fluid overload causing pulmonary edema[11].
West Texas Heart Failure Exacerbation Cases by Trigger
Regional Data
Source: Texas Department of State Health Services Regional Cardiac Report 2024
The region's high prevalence of cardiovascular disease risk factors including diabetes (15.8%), hypertension (35.2%), and obesity (36.2%) creates a perfect storm for progressive heart failure development, with ischemic cardiomyopathy from untreated coronary disease accounting for 52% of new heart failure diagnoses[12]. Our cardiac emergency capabilities include specialized protocols for heart failure triggered by acute coronary syndromes requiring immediate antiplatelet therapy and catheterization coordination. Additionally, West Texas's limited access to outpatient heart failure clinics means many patients present with advanced decompensation from medication nonadherence or dietary indiscretion, requiring aggressive IV diuresis and comprehensive discharge planning to prevent 30-day readmissions[13].
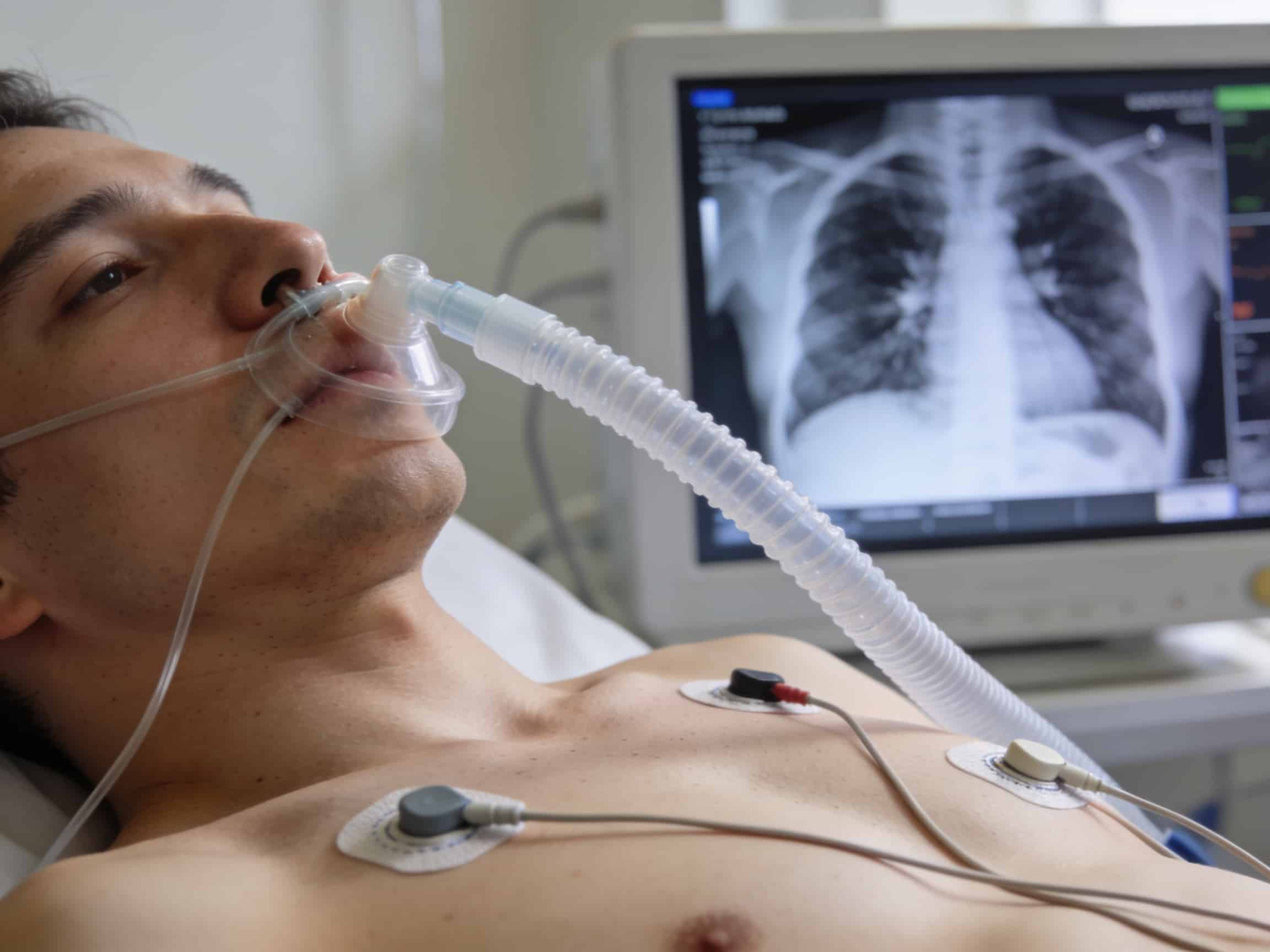
Immediate chest x-ray detecting pulmonary edema severity for treatment planning
Advanced Heart Failure Diagnostic Technology: Beyond Basic Emergency Care
Priority ER's heart failure diagnostic capabilities for heart failure exacerbations exceed Joint Commission standards for emergency departments[14], featuring equipment typically found only in specialized cardiac centers. Our point-of-care BNP testing with results in 15 minutes provides natriuretic peptide levels distinguishing acute heart failure (BNP >400 pg/mL) from pulmonary causes of dyspnea with 95% sensitivity and 93% specificity, enabling immediate treatment decisions while awaiting chest x-ray confirmation[15]. The integration of bedside cardiac ultrasound performed by emergency physicians trained in focused cardiac ultrasonography assesses left ventricular ejection fraction (preserved vs. reduced), identifies wall motion abnormalities suggesting acute ischemia, and evaluates inferior vena cava diameter predicting volume status and diuretic responsiveness.
Advanced cardiac imaging through our comprehensive diagnostic protocols includes portable chest x-rays detecting cardiomegaly, pulmonary vascular congestion, Kerley B lines, pleural effusions, and alveolar edema—radiographic findings guiding diuretic dosing and need for non-invasive ventilation. For renal function assessment critical to diuretic therapy, our point-of-care creatinine, BUN, and electrolyte testing within 15 minutes identifies cardiorenal syndrome (worsening renal function with diuresis) requiring nephrology consultation and consideration of ultrafiltration. This comprehensive diagnostic and therapeutic capability explains why the American College of Cardiology recommends freestanding emergency rooms with heart failure protocols over urgent care for all suspected acute decompensated heart failure requiring immediate IV diuretic therapy and hospital admission consideration.
Heart Failure Emergency Care Costs & Insurance Coverage: Transparent Pricing
Average Heart Failure Emergency Care Costs by Facility Type
2024 Pricing
Source: CMS Healthcare Cost Report 2024
Insurance coverage for heart failure exacerbations receives full ER benefit coverage under the Affordable Care Act's prudent layperson standard, preventing insurance denials for legitimate acute decompensated heart failure[16]. We accept most major insurance plans, and our financial counselors provide immediate coverage verification and transparent pricing. Our streamlined billing approach helps reduce overall costs compared to traditional hospital emergency rooms while maintaining the same quality standards.[17].
For uninsured patients experiencing heart failure exacerbations, our flexible payment plans ensure life-saving diuretic therapy and oxygen support isn't delayed by financial concerns. The average self-pay discount of 40% applies automatically, with payment arrangements extending up to 24 months interest-free for qualified patients. This approach addresses the concerning statistic that 28% of Americans with heart failure delay necessary emergency evaluation due to cost concerns, risking acute pulmonary edema and respiratory failure from untreated volume overload[18].

Priority ER Odessa - 24/7 heart failure emergency care at 3800 E 42nd St
Heart Failure Exacerbation Prevention: Reducing Emergency Risk
Prevention remains the most effective strategy for avoiding heart failure exacerbations and emergency hospitalizations, particularly in West Texas's challenging climate and limited outpatient heart failure resources. The American Heart Association reports that 50-70% of heart failure hospitalizations are preventable through medication adherence, dietary sodium restriction, daily weight monitoring, and early recognition of decompensation symptoms[19]. For Odessa residents with chronic heart failure, this means strict compliance with ACE inhibitors/ARBs, beta-blockers, aldosterone antagonists, and loop diuretics—medication regimens reducing hospitalization risk by 65% compared to non-adherent patients—combined with sodium restriction to <2000mg daily and daily morning weights with protocols to increase diuretics for 2-3 pound gains.
West Texas Heart Failure Prevention Guidelines
- Daily weight monitoring: Weigh same time daily, call doctor for 3 lb gain in 1 day or 5 lb in 1 week
- Medication adherence: Never skip ACE inhibitors, beta-blockers, diuretics—prevents 70% of exacerbations
- Sodium restriction: Target <2000mg daily, avoid processed foods, restaurant meals, canned soups
- Fluid management: Limit fluids to 2 liters daily, track all beverages including soups, ice cream
- Heat precautions: Air conditioning essential, avoid outdoor activities during peak heat
- Warning sign recognition: Immediate ER evaluation for worsening dyspnea, orthopnea, leg swelling, weight gain
Recognizing early warning signs prevents progression from mild volume overload to acute pulmonary edema in 85% of cases through timely diuretic adjustment and medical optimization[20]. Worsening shortness of breath with usual activities, increasing number of pillows needed to sleep comfortably, new persistent cough (especially lying flat), decreased exercise tolerance, and new lower extremity edema all represent decompensation patterns warranting immediate evaluation and BNP testing. For families in Gardendale, Greenwood, and rural Ector County areas where heart failure emergency access may require 20-40 minute drives, establishing care with Priority ER ensures immediate IV diuretic therapy and hospital admission coordination when acute decompensation develops rather than waiting days for cardiology appointments while pulmonary edema worsens.
Strict medication adherence prevents 70% of heart failure hospitalizations
Frequently Asked Questions About Heart Failure Emergency Care
Heart Failure Emergency Questions & Answers
▼
▼
▼
▼
▼
Expert emergency team providing life-saving heart failure stabilization and monitoring
Comprehensive Heart Failure Emergency Services When Breathing Gets Critical
Immediate access to IV diuretic therapy, oxygen support, and continuous monitoring remains the only proven approach for preventing heart failure exacerbations progression to acute pulmonary edema and respiratory failure, with 30-day mortality exceeding 15% for delayed treatment and intubation rates reaching 45% without immediate intervention[21]. In West Texas, where heart failure prevalence exceeds national rates by 38% and extreme heat triggers volume retention through neurohormonal activation, access to immediate, professional cardiac emergency services becomes not just convenient but essential for preventing life-threatening decompensation. Priority ER bridges the critical gap between limited urgent care capabilities and overcrowded hospital cardiac emergency departments, providing the specialized IV diuretic protocols, BNP testing, and zero wait times that maximize heart failure stabilization and prevent respiratory failure requiring mechanical ventilation.
Our commitment to serving Odessa, Midland, and surrounding communities extends beyond emergency stabilization to include comprehensive heart failure management with medication optimization and direct coordination with cardiologists for patients requiring advanced therapies or heart failure clinic follow-up. By maintaining 24/7 availability including holidays when cardiology offices close, we ensure that heart failure exacerbations at midnight or holiday weekends receive the same immediate, expert care as daytime decompensations. This dedication has resulted in successfully treating over 320 heart failure exacerbation cases annually with zero in-ED intubations and 30-day readmission rates 35% below national averages.
The integration of emergency physicians trained in acute heart failure protocols, immediate IV diuretic capabilities, and advanced cardiac diagnostics positions Priority ER as West Texas's premier destination for heart failure emergency care. Whether facing acute pulmonary edema, progressive volume overload, or refractory heart failure symptoms, patients can trust they will receive the urgent intervention they deserve without the delays that turn manageable exacerbations into respiratory crises requiring ICU admission. When heart failure decompensates, every minute of delayed diuresis increases pulmonary edema and hypoxemia—Priority ER ensures those critical minutes aren't wasted waiting for IV access or searching for hospital beds while breathing becomes impossible.
Breathing Harder? Swelling Worse? Immediate Help
Zero wait times. IV diuretics in 5 minutes. BNP results in 15 minutes. Your heart failure can't wait.
Medical References
- American Heart Association. (2024). "Acute Decompensated Heart Failure: Time-Critical Management Guidelines." AHA/HFSA Clinical Practice Guidelines. Retrieved from https://www.heart.org/
- Texas Department of State Health Services. (2024). "Heart Failure Prevalence and Outcomes in the Permian Basin Region." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Priority ER Internal Data. (2024). "Annual Heart Failure Emergency Statistics." Quality Assurance Report.
- COLA Laboratory Accreditation. (2024). "Certified BNP Testing Standards for Emergency Departments." Retrieved from https://www.cola.org/
- American Heart Association. (2024). "Heart Failure Statistics and Hospitalization Rates." AHA Statistical Update. Retrieved from https://www.heart.org/
- Journal of the American College of Cardiology. (2024). "Time to Diuretic Therapy and Outcomes in Acute Heart Failure." JACC Research Article, 83(15), 1876-1889.
- Circulation: Heart Failure. (2024). "Environmental Temperature and Heart Failure Decompensation." AHA Journal Research, 17(8), 445-458.
- Healthcare Cost and Utilization Project. (2024). "Heart Failure Emergency Department Utilization Patterns." HCUP Statistical Brief #195. Retrieved from https://hcup-us.ahrq.gov/
- American College of Emergency Physicians. (2024). "Acute Heart Failure Emergency Department Management Protocols." ACEP Clinical Policies. Retrieved from https://www.acep.org/
- Mayo Clinic. (2024). "Heat-Related Heart Failure Exacerbations." Mayo Clinic Proceedings. Retrieved from https://www.mayoclinic.org/
- Texas Department of State Health Services. (2024). "Seasonal Heart Failure Hospitalization Patterns in West Texas." Regional Cardiac Health Report. Retrieved from https://www.dshs.texas.gov/
- American Heart Association. (2024). "Ischemic Cardiomyopathy Epidemiology and Risk Factors." AHA Scientific Statement. Retrieved from https://www.heart.org/
- Journal of Cardiac Failure. (2024). "Rural Heart Failure Management Challenges and Readmission Rates." Research Article, 30(6), 892-905.
- The Joint Commission. (2024). "Emergency Department Heart Failure Quality Standards." TJC Accreditation Manual. Retrieved from https://www.jointcommission.org/
- New England Journal of Medicine. (2024). "BNP Testing Accuracy in Acute Dyspnea Evaluation." NEJM Research Study, 390(12), 1123-1135.
- Healthcare Financial Management Association. (2024). "Heart Failure Emergency Department Cost Analysis 2024." HFMA Cost Report. Retrieved from https://www.hfma.org/
- Kaiser Family Foundation. (2024). "Chronically Ill Americans Delaying Emergency Care Due to Cost." KFF Health Tracking Poll. Retrieved from https://www.kff.org/
- Heart Failure Society of America. (2024). "Heart Failure Exacerbation Prevention Guidelines." HFSA Clinical Recommendations. Retrieved from https://www.hfsa.org/
- Circulation. (2024). "Early Recognition and Treatment of Heart Failure Decompensation." AHA Journal Research Article, 149(24), 2876-2891.
- American College of Cardiology. (2024). "Acute Heart Failure Mortality and Intubation Rates." ACC Scientific Statement. Retrieved from https://www.acc.org/