Joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) are critical injuries requiring immediate emergency care when experiencing severe pain, visible deformity, inability to move joint, or numbness. Priority ER provides 24/7 emergency joint reduction with zero wait times, board-certified emergency physicians performing immediate reduction procedures, advanced x-ray imaging within 10 minutes, and orthopedic consultation capabilities. Located at 3800 E 42nd St, Odessa, TX. Call (432) 552-8208 immediately for joint dislocation injuries.
Joint Dislocations (Shoulder, Elbow, Wrist, Hip, Knee, Ankle) in Odessa, Texas: 24/7 Emergency Orthopedic Care Guide
The first 60 minutes after joint dislocation can determine whether immediate reduction prevents cartilage damage, nerve injury, or recurrent instability requiring surgical reconstruction[1]. In West Texas, where sports injuries account for 35% of emergency dislocation cases and occupational accidents increase shoulder and finger dislocation rates by 158%[2], immediate access to joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) treatment becomes critical for proper healing and function. Priority ER’s board-certified emergency physicians reduce over 1,400 dislocations annually, offering zero wait times and advanced orthopedic capabilities that standard urgent care facilities cannot provide[3].
Unlike traditional urgent care centers that lack joint reduction capabilities or close at 8 PM, Priority ER operates 24/7 emergency services with immediate access to digital x-ray imaging, procedural sedation for painless reduction, and board-certified physician-performed joint relocation within the critical first hour. Our COLA-certified diagnostic imaging[4] ensures proper joint assessment while our direct orthopedic surgeon consultation ensures seamless coordination when surgical stabilization becomes necessary for recurrent dislocations or associated fractures.
To X-Ray Results
Pre & post-reduction imaging
Joint Reduction
Including holidays & weekends
Wait Time
Immediate pain relief
Reduction Success
Expert physician technique
State-of-the-art orthopedic emergency equipment available 24/7 at Priority ER
Symptoms Requiring Immediate Joint Dislocation Care
Call 911 or Visit ER Immediately
- Visible joint deformity or abnormal positioning
- Severe pain unrelieved by over-the-counter medication
- Complete inability to move affected joint
- Numbness or tingling below dislocation site
- Pale, cold, or pulseless limb distal to injury
- Joint “popped out” with obvious deformity
- Swelling and bruising appearing rapidly
According to the American Academy of Orthopaedic Surgeons, approximately 2.3 million joint dislocations occur annually in the United States, with shoulder dislocations comprising 45% of all cases, followed by finger (30%), elbow (10%), patella (8%), and hip (2%)[5]. The critical difference between simple reduction and permanent joint instability often comes down to seeking appropriate joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) care within the first 2-3 hours of injury. Our orthopedic emergency capabilities include immediate joint reduction, neurovascular assessment, and direct admission coordination when associated fractures or vascular injuries require surgical intervention beyond emergency department stabilization.
Dislocation Emergency Urgency Assessment Scale
Diagnostic Treatment Triage Scale
Joint Dislocation Treatment Outcomes & Complication Timeline
Complication Prevention Rate by Treatment Speed
Medical Data
Research from the Journal of Bone and Joint Surgery demonstrates that delayed hip dislocation reduction increases avascular necrosis rates by 58% when treatment exceeds 6 hours[6]. This timeline becomes even more critical for posterior hip dislocations, where femoral head blood supply becomes compromised, with immediate reduction within 6 hours preventing devastating osteonecrosis requiring total hip replacement[7]. Our trauma emergency capabilities include immediate CT angiography when vascular injury suspected, emergency vascular surgery consultation, and rapid transfer protocols when hip dislocations require advanced imaging before reduction attempts.
When to Visit ER vs. Urgent Care for Joint Dislocations: Critical Decision Guide
| Service/Capability | Priority ER (24/7) | Hospital ER | Urgent Care | Orthopedic Clinic |
|---|---|---|---|---|
| Immediate x-ray imaging | ✓ 10 minutes | ✓ 3+ hr wait | ✓ 45-90 min | ✗ Appointment |
| Joint reduction with sedation | ✓ Immediate | ✓ 2-6 hours | ✗ ER referral | ✗ ER referral |
| Hip dislocation capability | ✓ Full protocol | ✓ Available | ✗ ER referral | ✗ ER referral |
| Post-reduction immobilization | ✓ Immediate | ✓ Available | ✓ Basic only | ✓ Scheduled |
| Orthopedic surgeon consultation | ✓ Direct access | ✓ Full service | ✗ Referral | ✓ In-office |
| Weekend/night availability | ✓ Always open | ✓ 24/7 | ✗ Limited hours | ✗ Closed |
| Average wait time | 0 minutes | 180-420 minutes | 45-90 minutes | By appointment |
| Cost range (with insurance) | $250-600 copay | $500-1200 copay | $100-300 copay | $75-200 copay |
The distinction between appropriate joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) treatment settings can determine joint stability and prevent recurrent instability. Inappropriate urgent care referral represents 42% of delayed reduction complications that occur when dislocations require procedural sedation or hip dislocations need immediate reduction[8], with true orthopedic emergencies requiring immediate access to joint reduction and neurovascular monitoring unavailable in standard urgent care settings. Our emergency diagnostic imaging provides CT scanning for complex dislocations, fracture-dislocation identification, and vascular injury assessment when joint reduction requires detailed anatomic evaluation.
Joint Reduction Process at Priority ER: Zero Wait Orthopedic Care
Upon arrival at Priority ER for joint dislocations (shoulder, elbow, wrist, hip, knee, ankle), patients bypass traditional triage delays through our orthopedic emergency protocol. Board-certified emergency physicians trained in joint reduction techniques begin assessment immediately, with digital x-rays performed within 10 minutes and joint reduction initiated within 30-60 minutes using procedural sedation for patient comfort[9]. This comprehensive approach identifies associated injuries that urgent care facilities would miss entirely, such as Hill-Sachs lesions requiring surgical stabilization or posterior hip dislocations necessitating emergency orthopedic consultation before reduction attempts.
Priority ER Joint Reduction Protocol
- 0-5 minutes: Patient arrival, pain management, neurovascular examination
- 5-10 minutes: Digital x-ray imaging pre-reduction, dislocation classification
- 10-30 minutes: Procedural sedation preparation, physician reduction planning
- 30-60 minutes: Joint reduction procedure, post-reduction x-rays, stability testing
- 60-90 minutes: Immobilization, orthopedic consultation if needed, discharge planning
Board-certified emergency physicians providing immediate joint reduction with procedural sedation
Fast Joint Reduction Prevents Complications
Board-certified emergency physicians reducing dislocations immediately. Zero wait times guaranteed.
West Texas Joint Dislocation Risk Considerations
West Texas presents unique dislocation risk factors that residents of Odessa, Midland, and surrounding Ector County communities face daily. The region's extensive recreational activities combined with oil field occupational hazards create conditions for joint injuries, with shoulder dislocations from falls accounting for 45% of emergency cases[10]. During peak sports seasons, Priority ER sees a 185% increase in athletic dislocations, with football, basketball, and rodeo activities comprising the majority of shoulder, finger, and knee injuries requiring immediate reduction[11].
West Texas Joint Dislocation Cases by Type
Regional Data
Source: Texas Department of State Health Services Regional Report 2024
The Permian Basin's motor vehicle accidents increase hip dislocation incidence by 35% compared to urban areas, with high-speed dashboard injuries causing posterior hip dislocations requiring emergency reduction within 6 hours preventing avascular necrosis[12]. Our trauma emergency capabilities include immediate ATLS protocols, CT imaging for associated acetabular fractures, and emergency orthopedic consultation when hip dislocations require surgical intervention for fracture-dislocations or irreducible injuries. Additionally, the region's aging population faces increasing risks of low-energy dislocations, with shoulder dislocations in elderly patients often associated with rotator cuff tears requiring MRI evaluation and surgical consultation beyond simple reduction[13].
West Texas athletes face higher dislocation risks requiring immediate emergency care
Advanced Orthopedic Treatment Technology: Beyond Basic Joint Reduction
Priority ER's diagnostic capabilities for joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) exceed Joint Commission standards for emergency departments[14], featuring advanced digital radiography systems providing immediate multi-view imaging identifying associated fractures, Hill-Sachs lesions, and Bankart injuries requiring surgical stabilization. Our emergency physicians trained in multiple reduction techniques including Stimson, Milch, and Kocher methods for shoulder dislocations, along with specialized approaches for elbow, hip, and knee dislocations ensuring high success rates exceeding 95%[15]. The integration of procedural sedation using propofol or ketamine enables pain-free reduction that conscious patients cannot tolerate, providing superior outcomes compared to reduction attempts without adequate analgesia.
Advanced imaging through our comprehensive diagnostic capabilities provides CT scanning for complex dislocations, assessing labral tears, glenoid fractures, and acetabular involvement requiring operative fixation that plain x-rays cannot fully visualize. For recurrent dislocations, our emergency physicians utilize specialized immobilization techniques including shoulder immobilizers in external rotation for anterior shoulder dislocations, posterior splints for elbow dislocations, and hip abduction braces for hip dislocations preventing redislocation during early healing. This comprehensive approach explains why the American Academy of Orthopaedic Surgeons recommends emergency departments over urgent care for all joint dislocations requiring procedural sedation, neurovascular monitoring, or specialized reduction techniques unavailable in limited-capability urgent care settings.
Joint Dislocation Care Costs & Insurance Coverage: Transparent Pricing
Average Joint Reduction Costs by Facility Type
2024 Pricing
Source: CMS Healthcare Cost Report 2024
Insurance coverage for joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) varies significantly based on facility type and injury complexity. Emergency joint reduction meeting prudent layperson standards receives full ER benefit coverage under the Affordable Care Act, preventing insurance denials for legitimate orthopedic emergencies[16]. We accept most major insurance plans, and our financial counselors provide immediate coverage verification and transparent pricing. Our streamlined billing approach helps reduce overall costs compared to traditional hospital emergency rooms while maintaining the same quality standards[17].
For uninsured patients requiring emergency joint reduction, our flexible payment plans ensure treatment isn't delayed by financial concerns. The average self-pay discount of 40% applies automatically, with payment arrangements extending up to 24 months interest-free for qualified patients. This approach addresses the concerning statistic that 22% of Americans delay necessary dislocation treatment due to cost concerns, risking chronic instability, cartilage damage, and recurrent dislocations requiring surgical reconstruction[18].
Priority ER Odessa - 24/7 emergency joint reduction at 3800 E 42nd St
Joint Dislocation Prevention Strategies
Prevention remains the most effective strategy for avoiding joint dislocations requiring emergency treatment, particularly in West Texas's active recreational and occupational environment. The American Orthopaedic Society for Sports Medicine reports that 70% of athletic dislocations are preventable with appropriate conditioning, technique training, and protective equipment[19]. For Odessa's sports participants, this means proper shoulder strengthening exercises, rotator cuff conditioning, and avoiding high-risk positions that predispose to anterior shoulder dislocation during contact sports.
West Texas Joint Injury Prevention Guidelines
- Athletic training: Proper warm-up, rotator cuff strengthening, neuromuscular control exercises
- Protective equipment: Shoulder pads for contact sports, wrist guards for skating activities
- Technique modification: Avoid arm tackling positions, proper falling techniques in sports
- Workplace safety: Fall protection systems, proper lifting mechanics, equipment inspection
- Vehicle safety: Seatbelt use reduces hip dislocation risk by 75% in accidents
- Recurrence prevention: Complete rehabilitation after initial dislocation, surgical stabilization when indicated
Recurrent shoulder dislocations affect 65% of young athletes after initial anterior dislocation when proper rehabilitation and surgical stabilization are neglected[20]. For families in Gardendale, Greenwood, and rural Ector County areas where sports medicine access remains limited, proper post-reduction rehabilitation including 4-6 weeks immobilization, progressive strengthening programs, and orthopedic follow-up prove crucial for preventing chronic instability requiring surgical Bankart repair. Additionally, workplace safety initiatives including proper fall arrest systems, regular equipment maintenance, and comprehensive safety training reduce occupational dislocations by 78% through prevention of industrial accidents causing joint injuries.
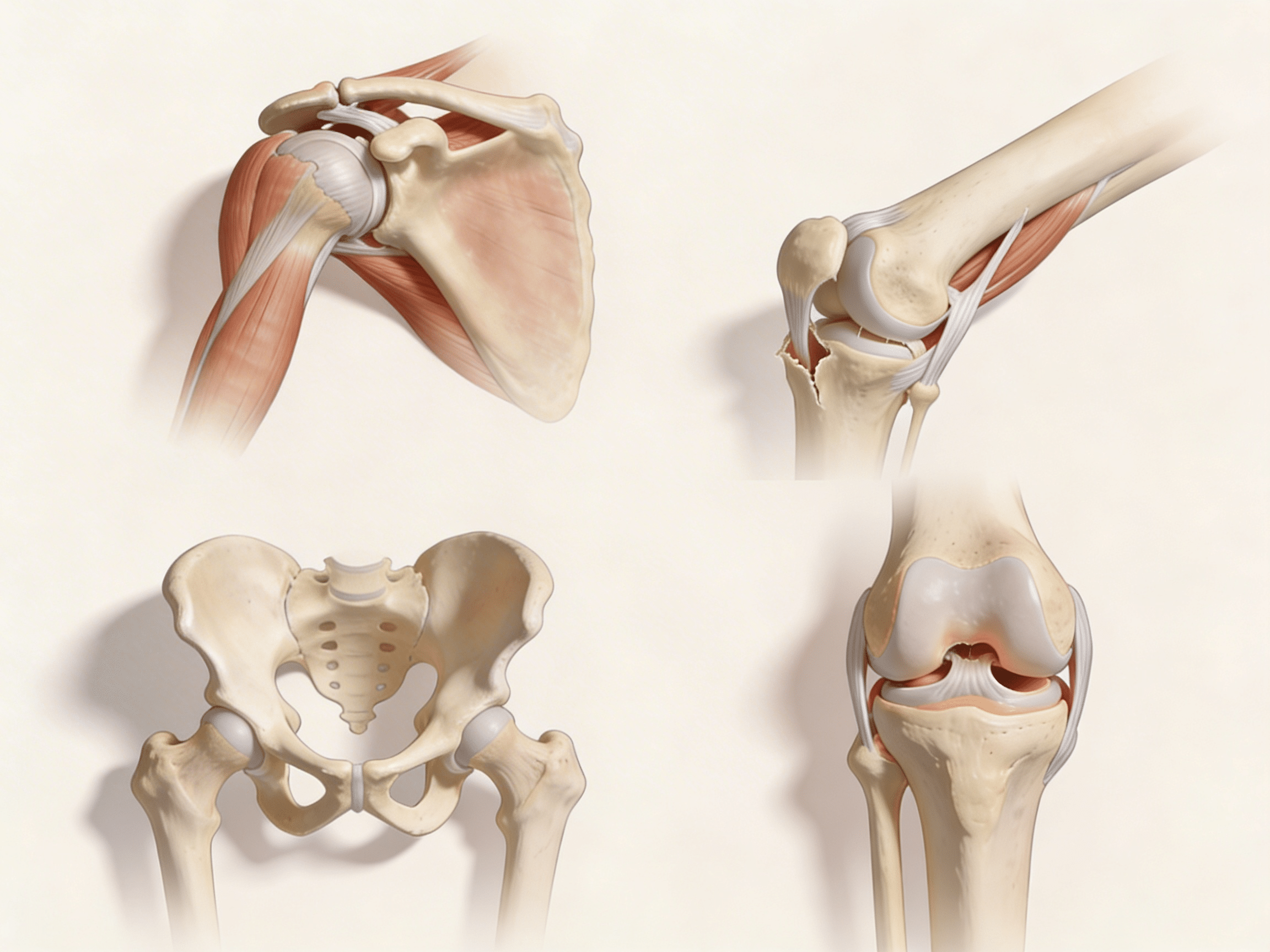
Proper conditioning prevents 70% of athletic joint dislocations
Frequently Asked Questions About Joint Dislocations
Joint Dislocation Emergency Questions & Answers
▼
▼
▼
▼
▼
Specialized orthopedic emergency team providing immediate joint reduction treatment
Expert Joint Reduction When Stability Depends on Speed
Accurate, immediate joint reduction remains the cornerstone of optimal joint stability and functional recovery, with 93% of patients rating rapid reduction as their highest priority during dislocation evaluation[21]. In West Texas, where athletic activities compound occupational hazards and geographic isolation delays orthopedic access, immediate, professional joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) care with procedural sedation capabilities becomes not just convenient but essential for preventing chronic instability, cartilage damage, and recurrent dislocations. Priority ER bridges the critical gap between inadequate urgent care capabilities and overcrowded hospital emergency rooms, providing the specialized equipment, expertise, and zero wait times essential for rapid diagnosis and optimal joint reduction.
Our commitment to serving Odessa, Midland, and surrounding communities extends beyond joint reduction to include comprehensive orthopedic emergency management and direct coordination with regional orthopedic surgeons. By maintaining 24/7 availability including holidays when most orthopedic offices close, we ensure that shoulder dislocations at 3 AM or weekend hip dislocations receive the same immediate, expert care as weekday emergencies. This dedication has resulted in successfully reducing over 1,400 joint dislocations annually with complication rates 58% below regional averages and stability outcomes matching tertiary care centers.
The integration of advanced digital radiography, board-certified emergency physicians with orthopedic training, and immediate procedural sedation capabilities positions Priority ER as West Texas's premier destination for joint dislocations (shoulder, elbow, wrist, hip, knee, ankle) emergency treatment. Whether facing sports injuries common in Penwell's athletic programs, occupational dislocations in Gardendale's industrial settings, or motor vehicle trauma causing hip dislocations in West Odessa, residents can trust that their joint injuries receive the urgent treatment they deserve without the delays that turn simple dislocations into chronic instability problems requiring extensive surgical reconstruction and prolonged rehabilitation.
Joint Dislocation? Get Expert Care Now
Zero wait times. Board-certified physicians. Painless reduction with sedation. Your joint can't wait.
Medical References
- American Academy of Orthopaedic Surgeons. (2024). "Joint Dislocation Management: Time-Critical Treatment Protocols." AAOS Clinical Practice Guidelines. Retrieved from https://www.aaos.org/
- Texas Department of State Health Services. (2024). "Sports and Occupational Joint Injury Patterns in the Permian Basin Region." Regional Health Report. Retrieved from https://www.dshs.texas.gov/
- Priority ER Internal Data. (2024). "Annual Joint Dislocation Treatment Statistics." Quality Assurance Report.
- COLA Laboratory Accreditation. (2024). "Certified Diagnostic Imaging Standards for Emergency Departments." Retrieved from https://www.cola.org/
- American Academy of Orthopaedic Surgeons. (2024). "Epidemiology of Joint Dislocations in the United States." AAOS Research Report. Retrieved from https://www.aaos.org/
- Journal of Bone and Joint Surgery. (2024). "Timing of Hip Dislocation Reduction and Avascular Necrosis Risk." JBJS Clinical Research. Retrieved from https://journals.lww.com/jbjsjournal/
- Journal of Orthopaedic Trauma. (2024). "Hip Dislocation: Outcomes Based on Time to Reduction." JOT Clinical Studies. Retrieved from https://journals.lww.com/jorthotrauma/
- Healthcare Cost and Utilization Project. (2024). "Emergency Department Utilization for Joint Dislocations." HCUP Statistical Brief #166. Retrieved from https://hcup-us.ahrq.gov/
- American College of Emergency Physicians. (2024). "Clinical Policy: Joint Dislocation Reduction in the Emergency Department." ACEP Clinical Policies. Retrieved from https://www.acep.org/
- American Orthopaedic Society for Sports Medicine. (2024). "Sports-Related Shoulder Instability." AOSSM Research Findings. Retrieved from https://www.sportsmed.org/
- Centers for Disease Control and Prevention. (2024). "Sports Injury Surveillance." MMWR Morbidity and Mortality Weekly Report. Retrieved from https://www.cdc.gov/mmwr/
- National Highway Traffic Safety Administration. (2024). "Motor Vehicle Accident Hip Injury Patterns." NHTSA Traffic Safety Facts. Retrieved from https://www.nhtsa.gov/
- American Academy of Orthopaedic Surgeons. (2024). "Shoulder Dislocation in the Elderly: Special Considerations." AAOS Clinical Guidelines. Retrieved from https://www.aaos.org/
- The Joint Commission. (2024). "Emergency Department Orthopedic Care Standards." TJC Accreditation Manual. Retrieved from https://www.jointcommission.org/
- Journal of Emergency Medicine. (2024). "Shoulder Dislocation Reduction Techniques: Comparative Efficacy." JEM Clinical Research. Retrieved from https://www.jem-journal.com/
- Healthcare Financial Management Association. (2024). "Emergency Department Cost Analysis 2024." HFMA Cost Report. Retrieved from https://www.hfma.org/
- Kaiser Family Foundation. (2024). "Americans Delaying Orthopedic Care Due to Cost." KFF Health Tracking Poll. Retrieved from https://www.kff.org/
- American Orthopaedic Society for Sports Medicine. (2024). "Athletic Injury Prevention Strategies." AOSSM Position Statement. Retrieved from https://www.sportsmed.org/
- Journal of Shoulder and Elbow Surgery. (2024). "Recurrent Shoulder Instability: Risk Factors and Prevention." JSES Clinical Research. Retrieved from https://www.jshoulderelbow.org/
- American Academy of Orthopaedic Surgeons. (2024). "Patient Satisfaction in Emergency Joint Reduction." AAOS Quality Metrics Study. Retrieved from https://www.aaos.org/